Download and print as a PDF (417kB pdf)
On this page
- What is Fentonâs repair?
- Why do I need this kind of surgery?
- What can I expect before the operation?
- What does the operation involve?
- What are the risks?
- What can I expect after the operation?
- What about going home?
- What about follow up?
- Are there any alternatives to this kind of surgery?
- Who can I contact with any concerns or questions?
- References and useful links
- Disclaimer
What is Fenton’s repair?
Fenton’s repair is an operation to correct tightness of the entrance of the vagina. This tightness might follow repair at the time of delivery or for prolapse.
Why do I need this kind of surgery?
Fenton’s repair is often recommended to relieve pain from the tight area, like during sexual activity, so as to improve the quality of life.
What can I expect before the operation?
You will be invited for pre op assessment, when the nursing staff will go through your hospital stay and explain your operation. Please do let us know about any concerns you have or if there is any information you think we should know about that will make your stay with us more comfortable.
You will need to make arrangements for your family, children or any other commitments that you have prior to coming in to hospital and to cover the length of your recovery.
On admission, the nursing staff will go through your stay on the ward again to ensure you feel comfortable whilst in the hospital.
You will see an anaesthetist and the doctor performing the surgery before you go to theatre. It is not unusual to feel anxious; the nursing staff will gladly discuss how you are feeling and talk you through your emotions.
If you have not already signed the consent form when your operation was agreed and booked, the doctor will go through it with you before you go to theatre.
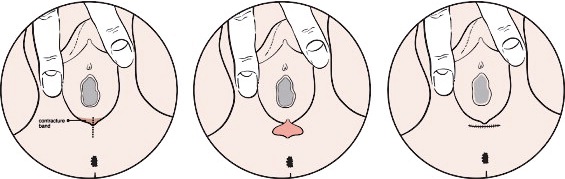
What does the operation involve?
The operation is done through the vagina. The tight scar tissue is divided, and at times removed. The vagina is then closed with sutures. A gauze pack may be left in the vagina, to avoid bruising.
The operation can be done under general anaesthesia, spinal anaesthesia or local anaesthesia, with or without sedation. The choice will depend on your preferences and other factors, such as whether you are breast feeding or not.
What are the risks?
There are risks with any operation but these are minor, as the operation is relatively minor. The main risks associated with these operations are:
Common risks:
- Postoperative pain. You will be provided with pain killers
- Wound infection, which may need antibiotics
- Wound bruising, breakdown and delayed wound healing
Uncommon risks:
- Venous thrombosis and pulmonary embolism (blood clot in leg / lung). These are reduced by elastic stockings and injections that thin the blood to prevent clots
- The operation may fail or the scar tissue may recur with time
- Bleeding requiring blood transfusion
- Return to theatre e.g. because of bleeding
In order for you to make an informed choice about your surgery please ask one of the doctors or nurses if you have any questions about the operation before signing the consent form.
What can I expect after the operation?
As you come round from the anaesthetic you may experience episodes of pain and / or nausea. Please let the nursing staff know and they will assess you and take appropriate action.
You may have a pack in the vagina, to stop any bleeding, or a dressing over the wound. The pack or dressing will be removed before you go home.
You will have a drip to give you fluids, though you will be able to eat and drink. It is not unusual to experience lower back pain and a feeling of fullness in your bowel and generalised discomfort when sitting. We use a pain score to assess your pain: 0 to 10: 0 = No Pain, 10 = Very Strong Pain.
Your nurse will be checking your blood pressure, pulse, respirations and temperature and monitor any vaginal bleeding. S/he will also ask you to move from side to side and to do leg and breathing exercises once you are able, this will help prevent any pressure damage, a DVT (deep vein thrombosis) or chest infection.
What about going home?
The operation is usually carried out as a day case. You will be encouraged to sit up and start to walk, when you feel comfortable. You will be able to go home when you are passing urine without difficulty.
Please feel free to ask questions about your operation and recovery at any time.
The nursing team will discuss your convalescence. To ensure you have a good recovery you should take note of the following:
What about follow up?
A follow up can be arranged, if required. This is usually organised for 12 weeks after surgery.
If you have problems, you can either contact your doctor or contact the hospital to arrange for an appointment or bring an arranged appointment forwards.
Are there any alternatives to this kind of surgery?
You will have been offered, and may have tried, local cream for lubrication and vaginal dilators before opting for surgery.
Who can I contact with any concerns or questions?
You should contact your doctor or the hospital if you notice increased temperature, wound swelling and / or pain, smelling discharge either from the wound or the front passage, blood in urine or motion, abdominal distension and / or failure to open your bowel.
If you have any problems or questions, you can contact:
Lewes Victoria Hospital
Urogynaecology Unit
01273 474 153
Ext. 2178
Monday to Friday
9:00 am to 5:00 pm
Princess Royal Hospital
Gynaecology Ward
01444 441 881
Ext. 5686
Royal Sussex County Hospital
Gynaecology Ward
01273 696 955
Ext. 4013
References and useful links
Guy’s and St Thomas’ NHS Foundation Trust patient information leaflet: Fenton’s repair
Leeds Teaching Hospitals NHS Trust patient information leaflet: Fenton’s repair
This patient information leaflet was prepared by Dr. Sharif Ismail, Consultant Subspecialist Urogynaecologist.
This information leaflet has been approved at the Clinical Governance and Safety and Quality Meetings of the Department of Obstetrics and Gynaecology as well as Brighton and Sussex University Hospitals NHS Trust Carer and Patient Information Group (CPIG).
Disclaimer
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.