Download and print as a PDF (356kB pdf)
On this page
- What is a laparoscopic colposuspension?
- Why do I need a laparoscopic colposuspension?
- What can I expect before the operation?
- What does the operation involve?
- What are the risks?
- What can I expect after the operation?
- What about going home?
- What about follow up?
- Are there any alternatives to having a laparoscopic colposuspension?
- Who can I contact with any concerns or questions?
- You should contact your doctor or the hospital if you notice:
- References/useful links:
What is a laparoscopic colposuspension?
Laparoscopic colposuspension is an operation done through key hole to avoid leakage of urine on coughing and sneezing. Stitches are used to support the bladder neck. The operation is carried out under general anaesthesia.
The laparoscopic (key hole) approach means less scarring and quicker recovery than open surgery.
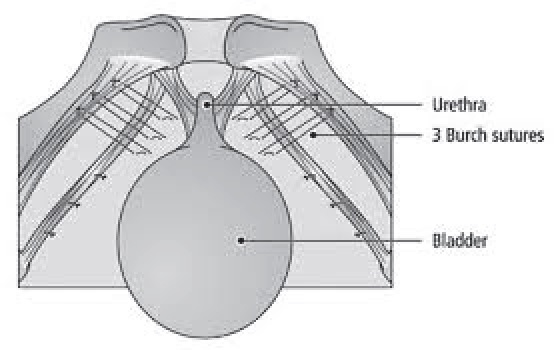
Why do I need a laparoscopic colposuspension?
Laparoscopic colposuspension is needed for stress incontinence of urine, which refers to leakage of small drops of urine on coughing and sneezing.
Surgery is carried out when conservative measures, such as pelvic floor muscle training, have failed.
What can I expect before the operation?
At your pre op assessment and on your admission day the nurse will go through your hospital stay and explain the operation. Please do let us know about any concerns you have or if there is any information you think we should know about that will make your stay with us more comfortable.
You will need to make arrangements for your family, children or any other commitments that you have, before coming in to hospital, and to cover the length of your recovery.
You will see an anaesthetist and the doctor performing the surgery before you go to theatre. If you have not already completed a quality of life questionnaire, you might be asked to do so before surgery. Likewise, if you have not already signed the consent form on booking, the doctor will go through it with you before you go to theatre.
You will be asked for permission to enter your data on the national database for continence and prolapse surgery. This is a quality control measure to compare the safety and effectiveness of such procedures at the hospital against other units in the country.
You will be given a quality of life questionnaires to complete and bring with you as you attend for follow up after surgery. This will enable assessing the benefit of surgery for you.
What does the operation involve?
The operation is done through a key hole approach. A small cut (1 cm) is made in the umbilicus (belly button), to introduce the laparoscope (tummy camera). If you had previous operation(s), this cut for may be made below the left side of the chest wall. Two additional small cuts (1/2 cm) are made, one on either side of your tummy. These cuts enable introducing instruments to do the operation.
What are the risks?
There are risks with any operation but these are small. The main risks associated with a laparoscopic colposuspension are:
Common risks:
- Postoperative pain, particularly shoulder tip pain. This is caused by the gas used to distend your abdomen being trapped under the muscle that separates the chest from the abdomen. Pain from this muscle is referred to the shoulder. This pain is usually mild and responds to pain killers. It often disappears within a day or two
- Initial difficulty in passing urine. This is usually managed by leaving the catheter (plastic tube) to drain the bladder for longer and you can go home with a leg bag for few days. Less commonly, patients may need intermittent self catheterisation for a short period of time
- Urinary tract infection, which may need antibiotics
Uncommon risks:
- Overactive bladder symptoms, such as frequency and urgency of passing urine may happen. These can be managed with medication
- Unmasking of weakness of the back wall of the vagina, leading to its prolapse. This may need pessary or surgery.
- Damage to the bladder and/or bowel, which will be repaired at time
- Late onset difficulty passing urine. This may manifest days or even weeks after being able to pass urine smoothly. The management is the same as initial difficulty passing urine, either by using a catheter with a leg bag and/or clean intermittent self-catheterisation
- Inability to complete the operation through the key-hole, which may necessitate laparotomy (open tummy) approach
- Venous thrombosis and pulmonary embolism (clot in leg/lung). These are prevented by elastic stockings and anticoagulants (injections that thin the blood to prevent a clot)
- Failure to improve or cure stress incontinence or its recurrence with time. This happens in less than 10% of cases on average. This will require re-assessment and might necessitate repeat surgery
- Hernia at site of entry
- Haemorrhage requiring blood transfusion
- Return to theatre because i.e. because of bleeding
- Wound infection, which may need antibiotics
- Wound bruising and delayed wound healing
In order for you to make an informed choice about your surgery please ask one of the doctors or nurses if you have any questions about the operation before signing the consent form.
What can I expect after the operation?
As you come round from the anaesthetic you may experience episodes of pain and / or nausea. Please let the nursing staff know and they will assess you and take appropriate action. You may have a PCA (Patient Controlled Analgesia) pump to control your pain. This is not common and will be discussed with you before the operation by the anaesthetist. The nurses will assess you regularly to ensure that the PCA is effective. We will use a pain score to assess your pain 0 to 10; 0 No Pain, 10 Very Strong Pain.
Your nurse will be checking your blood pressure, pulse, breathing and temperature and monitor the laparoscopic ports and any vaginal bleeding. S/he will also ask you to move from side to side and to do leg and breathing exercises once you are able. This will help prevent any pressure damage, a DVT (deep vein thrombosis) or chest infection.
The first 12 hours after the operation
You will have a drip attached but will be able to eat and drink once you are fully awake. Your drip will then be discontinued. You may also have a catheter to drain the bladder. You can expect pain and discomfort in your lower abdomen for the first few days after the operation. You may experience shoulder tip pain from the gas trapped under your rib cage. This is the gas used to distend your tummy during the operation and is common following laparoscopic (key hole) surgery. You will be given pain killers to alleviate this.
Day 1 after the operation
The nursing staff will assist with washing as necessary and encourage early mobilisation. We would normally expect you to sit out of bed and begin to walk around the day after your operation. The drip, drain and catheter are usually removed. You will be asked to pass urine in a jug and will have a scan to measure how much urine is left in the bladder. It helps to forget that you need to pass urine and drink and walk as you would normally do, and this is when your bladder is likely to work as normal.
You will have 2 to 4 small dressings on the cuts in your abdomen. These will be removed the day after your operation and you will be able to shower. You may experience trapped wind which can cause discomfort. Peppermint water, getting up and walking around will help this. You may also find it difficult to open your bowels at first. You can have mild laxatives to soften your stools and prevent constipation and straining.
What about going home?
You will be seen and assessed by the gynaecology team the following day to check on your recovery and decisions will be made about your care. This information will be shared with you. Please feel free to ask questions about your operation and recovery at any time.
The average length of stay following a laparoscopic colposuspension is 1-2 days. As you physically recover from your operation, the nursing team will discuss your convalescence. To ensure you have a good recovery you should take note of the following:
What about follow up?
You will be invited for follow up, usually at Lewes Victoria Hospital about 12 weeks after surgery. If you have problems before this you can either contact your doctor or contact the hospital to bring the appointment forwards. During this follow up appointment, your symptoms will be reviewed and you will be examined to assess wound healing. The frequency volume chart and quality of life will be checked.
Are there any alternatives to having a laparoscopic colposuspension?
You may decide not to have surgery. You will have had pelvic floor muscle training with a specialist physiotherapist before surgery is considered.
Alternative forms of surgery include:
- Burch colposuspension, which is the same operation performed abdominally (through a cut across the tummy)
- Autologus sling, an operation to support the urethra using a strip from the abdominal (tummy) wall
- Injection of synthetic material at the bladder neck
The use of tapes was paused, in line with national advice.
These can be discussed with your doctor.
Who can I contact with any concerns or questions?
You should contact your doctor or the hospital if you notice:
- Increased temperature
- Wound swelling and / or pain
- Smelling discharge either from the wound or your vagina
- Blood in urine or stools (poo), abdominal distension and / or failure to open your bowel
If you have any problems or questions, you can contact:
Lewes Victoria Hospital Urogynaecology Unit
01273 474 153
Ext. 2178
Monday to Friday
9:00 am to 5:00 pm
Princess Royal Hospital Gynaecology Ward
01444 441 881
Ext. 5686
Royal Sussex County Hospital Gynaecology Ward
01273 696 955
Ext. 4013
References/useful links:
Useful resources
The British Society of Urologists website: Colposuspension leaflet
Yourpelvicfloor.org leaflet: Colposuspension
If you do not understand this leaflet, we can arrange for an interpreter.
This information leaflet has been produced by Dr. Sharif Ismail, Consultant Subspecialist Urogynaecologist.
This information leaflet has been approved at the Clinical Governance and Safety and Quality Meetings of the Department of Obstetrics and Gynaecology as well as Brighton and Sussex University Hospitals NHS Trust Carer and Patient Information Group (CPIG).
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.