On this page
What is this information about?
This information describes exercises to do before and after you have had any kind of surgery to your spine.
These exercises include:
- Standing exercises
- Cervical (top of the spine) exercises
- Lumbar (lower spine) exercises
Reading this information, and doing these exercises, will help to support your recovery.
Standing exercises
Heel raises


- Hold onto something solid with one hand
- Raise heels off the floor
- Hold for 1 second
- Lower heels back down
- Repeat 10 times, rest and repeat
Squats

- Practise this exercise with hands hovering over bar
- Squat down and push bottom up
- Make sure your heels stay on the floor
- Repeat this up to 10 times
- Rest and repeat
Hip Extension

- Hold on with both hands
- Lift straight leg out behind you, make sure your toes remain facing forwards
- Complete this up to 10 times
- Complete the same on the other leg
- Rest and repeat on each leg
Hip Abduction

- Hold on with both hands
- Lift leg out sideways, make sure your toes remain facing forwards
- Complete this up to 10 times
- Complete the same on the other leg
- Rest and repeat on each leg
Marching

- For this exercise hold on with both hands
- Lift one leg up at a time as high as you can
- Do this for 1 to 2 minute(s)
- Rest and repeat
Side Stepping
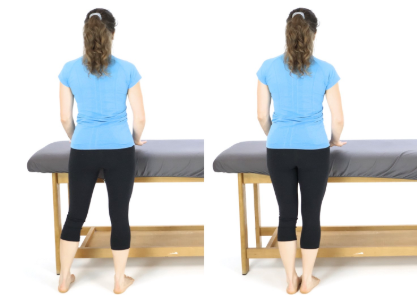
- Hold on to the rail with both hands
- Squat down slightly
- Sidestep sideways to the left
- Make sure you lift both feet!
- Repeat to the right
- Do this for 2 minutes
- Rest and repeat
- If you are able, try hover your hands over the surface to test your balance
Cervical Spine Exercises
Shoulder retraction. Repeat this 10 times.


Rotation to the right and left.


Forward flexion (looking down) and extension (looking up). Rotation to the right and left. Repeat 5 times.
Bring your chin to your chest, then rotate your head to the left or right side and nod your head 5 times to the right and then the left.
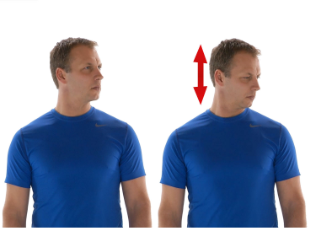

Chin tuck. Repeat this 10 times.


If you have increased pain following these exercises, please stop. The exercises can be repeated 3 times a day.
Lumbar Exercises

Heel Slides
- Slide your heel toward your buttocks while keeping it on the bed.
- Make sure you knee stays in line with your hip
- Move it as far as you comfortably can.
- Repeat as many times as possible until you feel tired
- Rest and repeat

Hip Abduction
- Slide leg outwards across the bed
- Keep toes up towards ceiling
- Slide leg back towards body
- Repeat as many times as possible until you feel tired
- Rest and repeat

Straight leg Raise
- Keep knee straight
- Lift leg straight up off the bed
- Hold for 3 seconds
- Repeat as many times as possible until you feel tired
- Rest and repeat 2 more sets

Clam.
Do
- this from 2 weeks after your operation
- Lying on your side with hips and knees bent
- Keep your ankles together and raise your top knee towards the ceiling
- Make sure you do not roll back when lifting your leg
- Repeat this 5 to 10 times
- Rest and repeat

Bridge
Do
- this from 8 weeks after your operation
- Squeeze your bottom
- Pull tummy in
- Lift bottom off the floor
- Hold for 3 seconds and SLOWLY lower
- Repeat this 5 to 10 times
- Rest and repeat
This leaflet is intended for patients receiving care in Brighton and Hove.
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Today’s research is tomorrow’s treatments. That’s why UHSx is proud to be a research-active Trust. Find out how you can get involved.
Visit our website www.uhsussex.nhs.uk/research-and-innovation/information-for-patients-and-public or scan the QR code: