Download and print as a PDF (893kB pdf)
Information for patients
On this page
- What is this information about?
- Why have I been given this information?
- What is coronary heart disease?
- What is angina?
- What is a heart attack?
- What should I do if I have chest pain or angina?
- Do
- What positive points should I remember?
- Do
- Your recovery and rehabilitation (rehab)
- Be aware
- Returning to work
- Driving
- Sex
- Do
- Do not
- Holidays and air travel
- Do
- Exercise
- Do
- Medicines
- Antiplatelets
- Useful contacts phone numbers:
- Which websites might I find useful?
What is this information about?
This information is about heart problems such as angina or heart attack. It explains:
- what has happened to your heart
- what tests and treatments you may have
- how to look after yourself and lower the risk of future problems
- where to get help and support.
Why have I been given this information?
It is likely that you (or your family member, friend or carer) have been given this information because you have come into hospital with heart problems. You may:
- have had chest pain, angina, or a heart attack
- been told you have coronary heart disease
- be recovering from any other heart condition.
Hospital is the safest place to check your heart and start any treatment that you need.
When you come into hospital with heart problems it is usual to feel frightened, anxious and confused. You may find it hard to concentrate and have lost your appetite.
Reading this leaflet and following the advice in it will help you:
- understand what happened and why
- know what to do if you get chest pain again
- recover safely and return to what you were able to do before
- reduce your chance of having another heart problem.
Give yourself time to read this information carefully. Work through it at your own pace and refer to it as you recover over the coming weeks. Write down any questions or worries you and your family may have. The doctors, nurses and cardiac rehabilitation (rehab) team will be happy to discuss them.
If you have questions, speak to the ward team or phone the cardiac rehab team:
Phone: 01273 446019 (Monday to Friday, 8am to 4.30pm).
This is not an emergency number. If there is no-one there to answer your call, please leave a message on the answer phone. We will get back to you as soon as possible.
Why did I get a heart problem?
To help you to understand why you have had a heart problem it is useful to know how the heart works.
Your heart is a muscle that pumps blood around your body. It needs its own blood supply which it gets through blood vessels called coronary arteries.
- The left coronary artery (LCA) splits into two branches called the ‘left anterior descending’ (LAD) and ‘circumflex’ (Cx).
- The right coronary artery (RCA) supplies the right side of the heart.
These main arteries divide into smaller branches as shown in the diagram below.
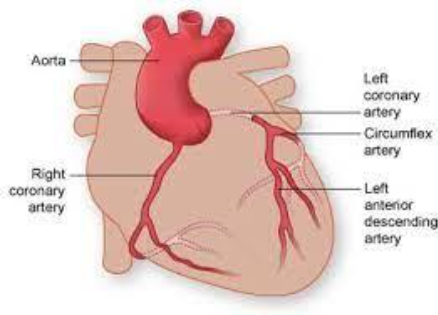

What is coronary heart disease?
Coronary heart disease happens when fatty material called plaque builds up inside the arteries.
Plaque is made up of things such as cholesterol, waste from your body’s cells and parts of your blood.
When plaque builds up in your arteries it makes them narrow and reduces blood flow. This can lead to your heart muscle not getting enough blood or oxygen to work as it should.
It can cause you to have:
- angina
- a heart attack.
- acute coronary syndrome.
Which of these you get depends on how narrow your coronary artery becomes.
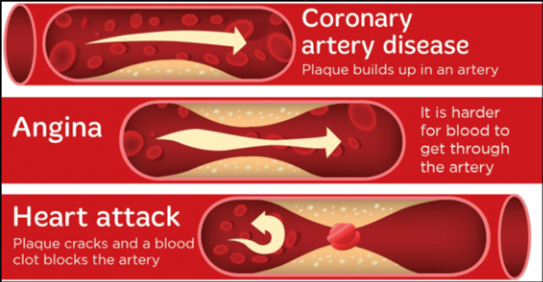
What is angina?
Angina is the name for a set of symptoms that you may get if you have narrow arteries and your heart has to work harder than usual. For example, this could be when you exercise or are stressed.
If you have angina you may feel:
- tightness or heaviness in your chest
- pain in your arms, neck, jaw, back or stomach
- shortness of breath, dizziness or feeling sick.
For further information see the British Heart Foundation’s “Understanding Angina” leaflet.
What is a heart attack?
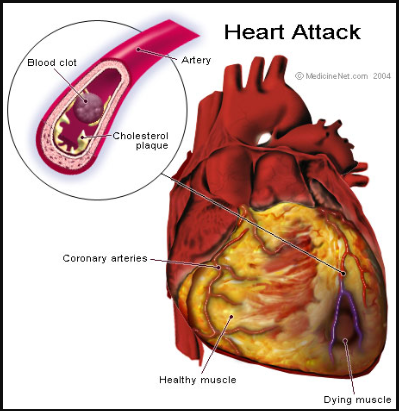
If an artery becomes partly or completely blocked, you may be told you have had a heart attack.
A heart attack is also known as a ‘myocardial infarction’ (MI). It happens when:
- a plaque inside the artery ruptures (suddenly bursts or tears)
- a blood clot forms to heal the rupture
- the clot reduces or stops the blood flowing to an area of heart muscle.
If:
- your artery is completely blocked and
- you do not get treatment to clear the blockage straight away
the area of the heart that gets its blood supply from that artery may be damaged forever. That part of the heart muscle may die and scar tissue forms over the following weeks.
Depending on the size of the affected area and where it is, the heart may not pump as strongly. This may mean you need extra treatment and take longer to recover.
More often:
- a heart attack does not cause permanent damage to your heart
- recovery is straightforward
What should I do if I have chest pain or angina?
If you have:
- been diagnosed with coronary heart disease and
- been prescribed GTN spray or tablets and
- have chest pain or symptoms such as:
- pain, tightness or heaviness (or any combination of these) in an arm or shoulder or in your neck, jaw, back or stomach or
- shortness of breath, dizzy or nauseous (feeling sick)
Do
- Use your GTN spray or tablet, under the tongue.
- Wait 5 minutes to see if your angina goes away. It is likely that your symptoms will have gone after this time.
- If you still have symptoms, take your GTN spray again.
- Wait a further 5 minutes.
- If the symptoms have not gone completely after 10 minutes and the 2nd dose of GTN do phone 999 straight away. Do not wait any longer before phoning.
- Chew one aspirin tablet (an adult dose of aspirin, 300mg) if you have one nearby and are not allergic to aspirin.
Be aware,
if you think you may be having a heart attack (even if your symptoms are not the same as those above) do phone 999 straight away.
How long might it take me to recover from a heart attack?
- If you have a minor (less serious) heart attack you may recover fully in 2 to 3 weeks
- If you have a moderate or major (more serious) heart attack it can take 6 to 8 weeks to recover.
How can you tell if I have coronary heart disease (CHD)?
We can tell if you have coronary heart disease (diagnose you with coronary heart disease) by:
- checking if the symptoms that you came into hospital with match those of CHD.
- a doctor examining you and checking for signs that you may have CHD
- looking at the results of your ‘heart trace’ (electrocardiogram or ECG). We will take several ECGs while you are in hospital.
- checking whether your blood levels of an enzyme called troponin show that your heart has been damaged. We will take several blood tests while you are in hospital.
What treatment might I get straight away?
You may get treatment straightaway to:
- relieve any pain or discomfort you may be in
- increase the blood flow through the narrowed artery
- reduce the work your heart has to do (how fast it has to pump).
What tests might I have to check how my heart is working?
You may have:
- echocardiogram (echo). This uses sound waves (ultrasound) to scan your heart chambers and valves
- coronary angiogram – shows if arteries are narrow or blocked
- myocardial perfusion scan – shows how much blood is supplied to your heart when you are at rest or exercising.
- cardiac MRI – a more thorough scan of your heart and how it is working.
What investigations (tests or checks) and treatments might I have?
You may have:
- Coronary angiogram or cardiac catheterisation
Cardiac catheterisation is an investigation not a treatment. It helps your doctors decide if you need further treatment by telling us:
- where and by how much your cardiac arteries are narrowed
- how well your heart’s pumping chambers and valves are working
- the blood pressure in your heart.
- Coronary angioplasty
This may be a PTCA (Percutaneous Transluminal Coronary Angioplasty) or PCI (Percutaneous Coronary Intervention).
If your angiogram shows you have narrowed areas in an artery which need to be treated to widen them, you may have an angioplasty.
In an angioplasty we place a small ‘balloon’ inside a blocked artery and inflate it to widen it and open it out. This means that more blood can flow to your heart muscle.
We may also place a stent (a short tube of metal mesh) in your artery. As the balloon is inflated the stent expands. It holds the narrowed coronary artery open, and the balloon is removed.
For further information see the British Heart Foundation’s “Understanding Coronary Angioplasty and stents“ leaflet.
- Coronary artery bypass graft (CABG)
For some people a ‘bypass operation’ (coronary artery bypass graft or CABG) is the best treatment. The surgeon makes new routes which bypass the damaged artery for blood to reach the heart. They may use a vein or artery from your chest, arm, or leg to do this.
For further information see the British Heart Foundations’s “Understanding coronary artery bypass surgery” leaflet.
What feelings and emotions might I experience while I am recovering from my heart condition?
Recovering from a heart problem takes time. Everyone feels and reacts differently, but you are likely to have emotional highs and lows. Many people feel:
- Shock. This often comes on early. You may feel emotionally ‘numb’ to other things that are happening and find it difficult to concentrate and fully understand what is happening.
- Fear, or that they are at risk (vulnerable). This can happen because you may feel that your life is out of your control. These feelings are likely to lessen as:
- you understand better what has happened to you
- you recover
- you regain more control over your life.
- Denial. Some people do not accept (deny) that the problem has happened. To start with this may help them to cope with the big changes in their lives. In the longer term accepting what has happened will help you to find ways to improve your situation.
- Anger. You may feel angry with hospital staff, family or friends and at the situation that you are in. You may also feel guilt. Talking with hospital staff and your visitors can help. Do try to deal with your anger as soon as you can so that you can then concentrate on your recovery.
- Depression. It is usual to feel depressed after a shock or any life-changing event which does not seem to be positive. Symptoms of depression can include:
- loss of appetite
- not sleeping well
- loss of interest in the outside world
- feeling weepy though you may not know exactly why. Crying can release tension and make you feel better.
- Acceptance. Once you can accept what has happened you can begin to move forward with your life. Your life can return to normal, or it may change. It can still be happy and rewarding.
Be aware,
your family and friends may also go through these emotions. Try to share your hopes and fears with them as this is often helpful.
What positive points should I remember?
- Heart problems do not mean that your heart is worn out
- Heart problems are not a sign that the body is wearing out
- Most people make a full recovery afterwards
- There are things that you can do to help prevent another attack
- It is usual to feel tired and weak for a while afterwards
- You are likely to get stronger every day.
What causes coronary heart disease (CHD)?
The things which cause CHD are not fully understood. We do know about some things which make it more likely that you may get CHD (risk factors for CHD).
Many of these can be controlled or reduced (modified). Making changes to your lifestyle can help improve your heart health a great deal.
There are other risk factors which cannot be controlled. These include things such as:
- a family history of heart disease
- your age
- your cultural background
- your gender.
These cannot be changed, even if you know about them (they are unmodifiable). Being aware of them can help you and your healthcare team to do things which can manage your overall risk.
There is a lot that you (and your healthcare team) can do to reduce ‘modifiable’ risk factors:
How can I reduce my risk?
Blood Pressure.
Keep your blood pressure within the target levels for you so that your heart does not have to work too hard. Make sure that you know your target level and have your blood pressure checked often. This could be every day until your blood pressure is controlled. After that you should have an annual check-up with your GP.
- The target level for people under 80 years old is less than 135 over 85 (<135/85)
- The target level for people over 80 years old is less than 145 over 85 (<145/85)
The first figure in the pair of figures in the target level is for your ‘systolic’ pressure. This is the pressure measured when your heart contracts (squeezes blood out).
The second figure in the pair is for your ‘diastolic’ pressure. This is the pressure when your heart relaxes again after it has contracted.
Your blood pressure should be measured when you are at rest. It should be lower than your target. ‘At rest’ means you are in a calm, relaxed state, both physically and mentally.
To make sure you are ‘at rest’ when you have your blood pressure measured:
- sit quietly in a comfortable chair with back support for at least five minutes before the measurement.
- keep your feet flat on the floor and legs uncrossed. Your arm should be supported on a flat surface, like a table, with the blood pressure cuff at the level of your heart.
- avoid activity. Do not talk during the measurement. Also, avoid exercising, drinking caffeine or alcohol, or using tobacco products for at least 30 minutes before taking the reading.
- empty your bladder. Have a pee before taking the reading.
Cholesterol
Lower your cholesterol levels. High cholesterol levels mean your arteries are more likely to fur up (get blocked).
It is likely that we will prescribe you medicine to lower your cholesterol. Do have a blood test to check your cholesterol level 1 to 2 months after you start taking this. The cardiac rehabilitation team or your GP will contact you to arrange this. You should then have at least 1 cholesterol test with your GP surgery each year after that.
The blood test that you should have is called a “full lipid profile”. This shows the levels of “good” (HDL) and “bad” (LDL) cholesterol in your blood. We aim for the “bad” cholesterol (LDL) to be less than 1.8 millimoles per litre (< 1.8 mmol/L).
Try following a ‘Mediterranean diet’ that is low in saturated fat and processed foods. This can help you to reduce the cholesterol levels in your blood.
Smoking
Do not smoke. There is no safe amount. Cigars, roll ups, pipes or cigarettes (with or without filters) all allow harmful chemicals into your blood. They damage the lining of your arteries and increase the chance that you will have further heart problems.
There is lots of help that you can get to help you to stop smoking. When you are in hospital a tobacco dependency advisor will see you to offer support to help you to quit. They can advise you on nicotine replacement therapy, e-cigarettes or vaping and medicines that can help.
They can also refer you to ‘Smoke Free West Sussex’ who can support you after you leave hospital.
The cardiac rehab team can also offer help when you are back at home by, for example, providing nicotine replacement therapy. They can also refer you to Smoke Free West Sussex.
If you need help to quit, please see the useful contact numbers at the back of this book.
Diabetes
Having diabetes increases your risk of heart problems.
If your HbA1c (‘blood glucose’ or ‘blood sugar’) reading is:
- 42 to 47mmol this means you are pre-diabetic. You have a higher chance of developing diabetes.
- 48mmol or higher this means you are diabetic.
To lower your risk, try to keep your blood glucose levels within the range that you have been advised. For many people the most effective way to reverse being pre-diabetic or diabetic is to lose weight.
Exercise
Stay active. Do try to get at least 150 minutes (2 and a half hours) of exercise every week. This should be ‘moderate intensity’ exercise. Brisk walking is a good thing to start with and build on. Your cardiac rehab team can advise you how to exercise safely and sensibly.
You do not have to do 150 minutes of exercise in one session. You could try breaking this up into 30 minutes of exercise on 5 days of the week. For some people, doing even shorter sessions than this, but doing them often, may suit them better. Regular physical activity improves your fitness and reduces your chance of having further heart problems.
Weight
Keep to a healthy weight. It is important that you are a healthy weight for your height. If you are overweight (you have a Body Mass Index of over 25 (BMI >25), this puts more strain on your heart.
A 10% weight loss (for example losing 11kg if you weigh 110kg) can improve cholesterol level and reduce your blood pressure and chance of having type 2 diabetes.
Waist
Keep your waist measurement in the ideal range for you. You are more at risk of heart problems if you carry more weight around your waist (you are ‘apple’ shaped with a larger tummy).
Measure around your waist at the widest part (this might not be where the waistband of clothing sits). Compare it with the waist measurements below and try to keep your waist measurement in the ideal range.
| Male | Female | |
| Ideal | Under 37 inches (94cm) | Under 31.5 inches (80cm) |
| Worrying | 37 to 40 inches (94 to 102cm) | 31.5 to 34.5 inches (80 to 88cm) |
| High risk | Over 40 inches (94cm) | Over 34.5 inches (88cm) |
Diet
Eat well. Choose fruit, vegetables, wholegrains, pulses, lean meat and fish (the ‘Mediterranean diet’). Cut down on salt, animal fats and processed foods.
Alcohol
Keep to less than 14 units each week and have 2 alcohol‑free days. A pub measure of spirits is 1 unit, a 250ml glass of wine is around 3 units and a pint of medium strength beer is 3 units.
It is ok to drink in moderation but be aware that alcohol is high in calories.
Stress
Stress has not been proved to cause heart problems but if you have a heart condition it does not help your situation. Try to avoid stress and use coping methods for when you are stressed.
When, and how, should I start to work on reducing my risk?
Start to look at your lifestyle and make changes to lower your risk and improve your health straight away.
- It is likely that you have recognized some changes you can make already
- Some people may not recognize that they have any risk factors
- For some people it is not clear why they have heart disease
- It is still important for everyone with heart disease to do what they can to improve their health and reduce their chances of having further heart problems.
Do
- Use the action plan below to identify the things that you think are your risk factors and how you might reduce your risk
- Ask your GP practice nurse or the Cardiac Rehab Team for further information or help to complete your action plan if it would help you.
Risk factor action plan
Use this to track how you are doing in improving your risk factors for heart disease and improving your heart health. (Please print off the PDF version at the top of this leaflet to fill in the form.)
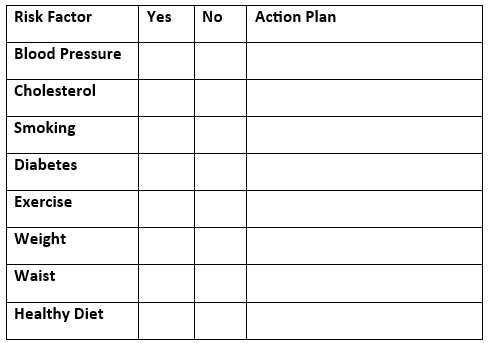
Where can I find further information that could help me to understand and reduce my risk factors?
You can find free information that may help you to understand and reduce your risk factors on these web-sites.
British Heart Foundation (BHF) Heart UKYour recovery and rehabilitation (rehab)
How long will I be in hospital and how active might I be during my stay?
The length of your stay will depend on:
- what checks we need to do to see how you are (tests and investigations)
- what treatment you need.
If the doctors think you need further investigations, you may be in hospital for longer.
At first you may be resting in bed but slowly, over time, you will be able to be more active until you are fully independent again. The doctors and nurses caring for you will advise you daily on how much you can do.
While you are recovering in hospital you will not be able to be very active. You are likely to be resting a lot of the time.
It is best for you and your heart if you become more active within a few days, if you are feeling well enough and have no symptoms. Too much time in bed is not good for you and will not help you to recover.
Be aware
stop any activity on the ward that causes you:
- chest pain, tightness or heaviness
- dizziness
- to feel breathless
- to feel very tired (fatigued).
Tell a member of staff straight away about your symptoms
What happens when I go home?
You are likely to feel tired for the first few days after you go home. This is usual as you have done very little during your stay in hospital.
You may feel or notice different sensations in your chest. This is often because you are likely to be thinking about and notice your chest more.
If you are worried about any symptoms or have any questions do phone us to get advice which is right for you. Phone: 01273 446019
Once you are back at home, slowly build up the amount of activity that you do.
Walking is the best activity to do when you are first recovering from a heart attack. Build your walking pace and distance up slowly. Walk at a pace which is:
- comfortable for you
- means you can talk without feeling breathless while you walk.
Who will oversee my healthcare once I am back at home?
You will be under the care of your GP once you go home from hospital. They will have your ‘discharge summary’ from the hospital. This tells your GP about your heart condition, what treatment you had in hospital and what further checks on your condition you may need.
Do try to make an appointment, which should be within 2 weeks of you coming home, to see your GP.
How do I get the medicines that I need once I go home?
Before you leave the hospital, we will give you enough of any medicines that have been prescribed for you to last for 4 weeks. Please order repeat prescriptions from your GP surgery. Do this far enough in advance that you do not run out.
Ask friends or family to remind you which medicines to take and when to take them until you have got used to what you need to take.
If you pay for your prescriptions, you could set up a prepayment certificate which means that if you need a lot of medicines the cost is likely to be lower for you. You can find further information at https://www.nhsbsa.nhs.uk/help-nhs-prescription-costs/nhs-prescription-prepayment-certificate-ppc

How can cardiac rehabilitation (rehab) benefit me and how can I get help from the Cardiac Rehabilitation Team?
Having cardiac rehab after you have had heart problems can greatly improve your:
- wellbeing and confidence
- understanding of your heart problem
- physical activity and fitness
- ability to cope.
Having cardiac rehab also means that you are less likely to have to go back into hospital because of a heart problem.
Access our online information sessions via the following link: https://www.uhsussex.nhs.uk/services/cardiology/cardiac-rehabilitation-at-worthing-hospital/
or use this QR code:


After you have gone home the Cardiac Rehab Team will contact you to offer you an appointment with them to
- check what rehabilitation would be right for you
- advise you on a cardiac rehab programme designed for you which will help you to recover. This may include gym exercise sessions, home-based exercise and online options.
Please contact the Cardiac Rehab Team for further information. Phone: 01273 446019. Do not use this line for emergencies.
When you have finished your cardiac rehab programme we will:
- advise you on how you can maintain your fitness, or improve it, in the longer term
- give you details of exercise facilities near your home.
What advice can I follow to guide returning to more activity once I’m at home?
How soon people are ready to return to doing the things that they used to is different for everyone.
- Progress slowly to doing more activity as you feel it is comfortable and safe for you to do so.
- You are likely to have days when you feel more able to do physical exercise and others when you do less. Pace yourself to avoid getting too tired.
- If you are finding it difficult to progress contact the Cardiac Rehab Team who can support you with this.
Try to progress through the stages of activity listed below. You may be able to move through the stages quite quickly. For example, you might work through two stages in a week. It may take longer so you spend a week or more on one stage.
Be aware,
if you have chest discomfort, unusual tiredness or are short of breath when you are doing any of the activities in any of the stages do:
– stop the activity
– speak with your GP or Cardiac Rehab Team about your symptoms and what you were doing when you had them.
Stage 1.
When you first come home continue the same routine of activities as during your last few days in hospital. If it feels comfortable, it is ok to use the stairs but try not to do this unless you need to.
Try doing any of these activities:
- Personal hygiene, such as washing and dressing
- Washing up
- Laying the table
- Basic food preparation, such as making a cup of tea or a light snack
- Desk-work (reading, typing, writing)
- Board or card games
- Craft work, such as sewing, knitting, or making model aeroplanes
- Walking around the garden
- Walking programme. See the section on walking further on in this information.
Stage 2.
- Light housework such as dusting
- Shopping
- Playing a musical instrument
- Using light hand and power tools
- Walking up a slight incline
- Light garden work such as weeding or planting small plants
- Golf (putting only)
- Sexual activity such as sexual intercourse
Stage 3.
- Housework such as sweeping, doing laundry or cleaning windows
- Light DIY and painting (no ceiling or high ladder work)
- Golf (pitch and putt, no driving)
- Garden work (no digging)
- Walking a dog.
Advice for partners and carers
It can be very worrying for you when your partner is in hospital with a heart condition and when they are recovering.
They may be:
- anxious and grumpy
- taking some time to come to terms with their condition and trying to cope in different ways
- trying to make big changes to their lifestyle
How can I help my partner when they come home from hospital?
- Be supportive and understanding
- Try to let them make their own decisions
- Help them make changes gradually and accept that they cannot do everything as soon as they come home
- Help them to regain confidence that they may have lost after their stay in hospital. For example, if they go for a walk, go with them.
- Talk with them about how you both feel and listen to them
- Allow each other some time and space alone
- Help them to take any new medicines in the right dose and at the right time. You may need to remind them to take their medicines and check that they have done so.
- Try to spend time at home with them. This is most important in the first few days after they come home but you do not need to stay in with them all the time. You also have to get back to daily life, including any work that you do.
- Explain to small children or grandchildren that you have that your partner may not be able to lift them up or run-around with them. Your partner can still do things with them such as sitting with them to play more gently or read a story.
Be aware, recovery from a heart condition can put pressure on a relationship. If you had problems before, they may be made worse. Do deal with any relationship problems separately from the recovery. Do try to talk. If you cannot, you may need to get further support from counselling.
Returning to work
What do I need to think about, and do, before I return to work?
You are likely to want to return to work as you recover. Many people can return to doing the work that they did before their illness. For others, the type of work that they did means this is difficult or not possible.
Talk with:
- your GP about returning to work.
- your employer about your job tasks and hours. See if you can, for example, do less hours or less strenuous or stressful work when you first return and build up to your previous levels over time.
If there are things about your work which may have contributed to your heart problem ask if there are things that your employer can do to change them.
- your family about how work, or not working, might affect your lives and your health
Be aware that although the people you work with will be concerned about you, they may soon forget that you were in hospital. They may expect or ask that you do things at work that you are not yet ready to do. Do tell people at work if something is too much for you at that time.
Avoid making a hasty decision about changing or giving up your job.
Please ask your hospital doctor if you need a sick certificate (fit note or doctor’s note) to cover your hospital stay. After that your GP will give you any further certificates.
Driving
What do I need to know about returning to driving?
- How soon you can return to driving depends on your diagnosis. Do check this with a ward staff member, the cardiac rehab team or your doctor.
- You do not need to tell the DVLA about your heart condition unless you hold an HGV (heavy goods vehicle), PCV (passenger carrying vehicle) or PSV (public service vehicle) licence.
Be aware, if you have an HGV, PCV or PSV licence you will need to have some tests as an outpatient. Depending on the results of these you may, or may not, be able to keep your licence.
Do not drive HGVs, PCVs or PSVs until your hospital doctor or GP has told you that you can.
- You must not drive if you have symptoms of angina while you are at rest or while you are driving. You can start driving again when your symptoms are well-controlled.
- Do not return to driving too soon even if you are an experienced driver. It can be stressful and tiring.
- Tell your insurance company about your heart condition.
Check with them that the terms of your policy will not be changed. Your current insurance company may try to increase the amount that you pay for your insurance or offer reduced insurance benefits. If so, check for better deals with other companies
The British Heart Foundation or the Cardiac Rehab Team can give you information about companies who may be likely to give people with heart conditions better terms.
Sex
How soon might I be able to have sex again?
There are no rules about when you start having sex again. It depends on how you and your partner feel but do try to wait for at least 2 weeks after going home. Both men and women who have had a hospital stay for a heart condition should allow their partner to do most of the ‘work’ to start with.
- There is only a very small chance of having a heart attack when you are having sex
- Having sex only makes your heart work as hard as climbing two flights of steps or walking a mile (on the flat) in 20 minutes.
How might I and my partner feel about having sex?
It is usual for your emotions to be disturbed after your stay in hospital. This might affect how you feel about sex. You and your partner may both lack confidence, feel nervous about having sex again or simply not feel like it.
This is likely to pass with time.
To help you return to your usual sexual activities:
Do
- give each other extra love and reassurance
- be honest with each other about how you are feeling
- be patient and sensitive to each other.
- talk with each other about your desires, hopes and worries about returning to having sex.
- talk with your doctor about any problems you are having getting back to your usual sex life. Ignoring them can make them worse and cause stress in your relationship with your partner.
Do not
- expect too much of each other.
- be alarmed if you have disappointments in the early stages. For example, if you are impotent, have erectile dysfunction or unable to have sex in the way you would wish to. Talk to your partner about this and maybe try again later.
Impotence may be the result of stress but could be related to medicines that you’re taking.
If you usually take medicines for erectile dysfunction do not start taking them again until you have talked about this with your GP or the Cardiac Rehabilitation Team. They may react with your heart medicines.
What practical advice about having sex should I follow?
- Try positions which will exert you less. This might be a side-to-side position. Go on top or below as you prefer and according to how much you feel it will exert you.
- Build up slowly to sexual activities that will exert you more. If you find sexual activities bring on your angina, take a GTN tablet or spray before you start.
- Allow plenty of time to recover from sex. Avoid heavy work afterwards.
- Avoid sexual activity:
- that makes you anxious
- when you are tired or tense. Choose times when you are relaxed and comfortable.
- for 2 hours after eating a heavy meal
- Do not have sex in a room which is too hot.
Holidays and air travel
Can I go on holiday after I come home from hospital?
A holiday can help you to recover but it is best not to take one for the first 4 to 6 weeks after you come home from hospital, especially if you have had a heart attack.
Holidays can be relaxing but may also cause some stress.
What should I do if I do go on holiday?
- Plan your trip carefully and allow plenty of time to get where you are going
- Stop at least every 2 hours for a break and to move around on long car journeys
- Get help with your luggage
- Get travel insurance. Make sure it provides you the cover for medical and other expenses that you may need. This is especially important if you are travelling abroad.
- Take out medical insurance when, or very soon after, you book your holiday.
- Talk with your GP or heart specialist doctor about any travel or holiday plans you have or if you have already booked a holiday. They will be able to advise you about whether you have recovered enough to be safe on your holiday and to fully enjoy it.
- Talk with your GP about what cover you may need and what to include in the health declarations on your insurance application. These can be very detailed and will be checked if you make a claim.
- Get further information on finding the right insurance for you from the BHF if you need it. See contact details later in this information.
What do I need to know about air travel?
Different airlines will have different advice and rules about flying if you have a heart condition. Check this before you book a holiday or fly. You can get further advice on flying from the Cardiac Rehabilitation Team.
Do
- consider not flying until you are fully recovered
- contact the airport or airline well before your trip to tell them if you need a wheelchair or buggy in the airport
- reduce the chance that you may get a blood clot (DVT) in your legs by:
- walking in the aisle on any flight over 2 hours. If it is difficult to walk in the aisle do foot movements instead. Raise your toes while keeping your heels on the ground for around 5 minutes every half hour.
- asking if your airline provides information about in-flight exercises that you can do. Most airlines can provide this.
- drink plenty of water throughout the day and at night. Avoid alcohol and limit caffeinated drinks
- make sure you have a copy of your prescription with you. Take enough medicine with you to last through your holiday and some extra in case of delays Try to have a supply of medicine in your hand luggage as well as in your luggage in the hold.
GTN spray in a pressurized container is safe to use on your flight. Check with your airline if it is ok to carry it in your hand luggage, especially at times of increased security.
Exercise
What kind of exercise should I take to help my recovery?
Getting the right kind of exercise will help you to recover.
The best kind of exercise for you to do is exercise that you enjoy and that is safe for you. This might be, for example, walking, cycling, dancing, or going to the gym. You do not need to be athletic or sporty to get the exercise you need.
Any exercise that moves both your arms and legs will help to strengthen your heart. If you have any questions about exercise do ask the Cardiac Rehabilitation Team for advice or support.
What do I need to know to help me to exercise safely?
- Weather. Avoid exercising in very cold weather, a strong wind or breeze, or when it is very hot. This might be, for example, on a chilly morning or evening or in midday heat. Walking in these conditions could cause you to have breathlessness or tightness, heaviness or pain in your chest.
- If you do have to go out in the cold, try wrapping a scarf around your nose and mouth to warm the air going into your chest.
- Clothes. When you exercise, always try to wear:
- comfortable, loose, clothes
- several light layers which you can take off and put on as you warm up or cool down.
- shoes which are comfortable, supportive and have good grip.
- Smoking and drinking alcohol. Try to give up smoking completely. If you cannot, do not smoke just before you exercise as this can alter your heart rate.
- Avoid drinking alcohol before you exercise.
- Meals. Do not have a heavy meal before a brisk walk or doing any exercise. Wait at least 1 to 2 hours after a heavy meal. This is because your heart sends lots of blood and oxygen to your stomach in this time to help to digest your food. Your heart would have to work even harder to supply blood to your muscles if you were to exercise.
- ‘Warm up’ and ‘cool down’ routine. Take the first part of your session slowly. This avoids putting your heart under too much strain at first and lets your heart, muscles and joints ‘warm up’ to your exercise. Your heart can build-up to beating faster and stronger. ‘Cool down’ from your session by exercising more slowly towards the end of it. This is so your body can adjust to you stopping.
Exercise within your limits and do not exercise to prove to others that you are fit.
Be aware:
If you get so out of breath when you exercise that you cannot talk, you are doing too much.
Stop exercising straight away if you:
-get chest pain or tightness in your chest
-feel tired or unwell
-feel dizzy or sick (nauseous)
-feel cold or clammy
-have a racing heart or heart flutter (palpitations)
Do
- contact your GP or let your cardiac rehab team know if you have any of these symptoms when you are exercising.
How hard should I exercise and how much time should I spend exercising?
Try to exercise for 150 minutes (2 ½ hours) a week. This will help to strengthen your heart. Break this up into shorter sessions if this is easier for you. For example, you could do 5 sessions of 30 minutes each. If 30 minutes is too long for you to exercise without a break, try doing 3 sessions of 10 minutes each. This will help build up your stamina and strength so you can do longer sessions.
Aim for moderate effort which makes you feel warm and a bit out of breath but still able to talk.
Effort guide: which
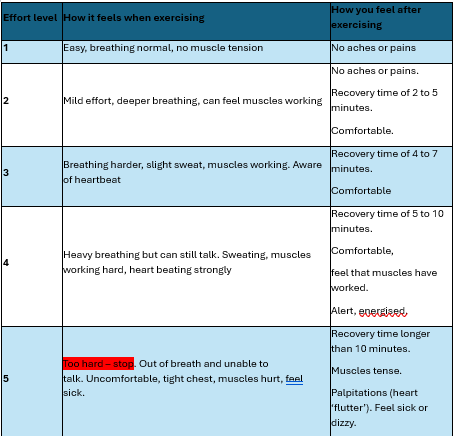
Be aware:
-you should not reach level 5.
-stop exercising straight away if you have symptoms of angina
-wait until the angina goes away before starting to exercise again at a lower level
-if the pain does not get better when you rest use your GTN spray or tablets
-if your angina seems to be coming on more often or takes longer to go away do contact your GP.
Aim for level 2 to start with and as your body gets used to exercising build up to level 3 or 4.
Be aware,
the table is only a guide to what you may be able to do. Everyone will progress through the stages at a different rate.
What exercise plan should I follow?
Follow the stages of activity in the table below. This will help you, and us, to check your progress.
The cardiac rehabilitation team will help you to find a level and type of exercise that is right for you.
- Work through the stages at your own pace. For example, you might work through two stages in a week. It may take longer so you spend a week or more on one stage.
- Start by building up the amount of time you spend exercising as shown in the table. Once you can exercise easily for the time suggested, increase the speed at which you exercise.
| Stage | Minutes of exercise | Times per day |
| 1 | 5 | 1 to 2 |
| 2 | 10 | 2 |
| 3 | 15 | 2 |
| 4 | 20 | 1 to 2 |
| 5 | 25 to 30 | 1 to 2 |
| 6+ | 30 to 40 | 1 to 2 |
You could track your progress through the stages by keeping a diary of:
- how much exercise you are doing
- how often you exercise
- how you feel when you exercise. For example, sweaty, out of breath, warm, or in pain.
- anything else that you think would help you.
Be aware,
once you are confident and able to exercise it is important to continue to exercise in the long term.
For current details about gyms, exercise groups and schemes in your area that can help you and motivate you to stick with exercising and keep up your good work, contact:
the cardiac rehabilitation team. Phone: 01273 446019
We can recommend exercise venues who provide a cardiac trained instructor.
Medicines
We may give you new medicines to start taking while you are in hospital. You must continue to take them when you go home unless your GP or hospital doctor tells you otherwise.
Before you leave the hospital, we will give you enough of any medicines that have been prescribed for you to last for 4 weeks.
Please do:
- order repeat prescriptions from your GP surgery
- order these far enough in advance that you do not run out
- carry a list of the medicines that you are taking with you at all times.
If you pay for your prescriptions, you could set up a prepayment certificate which means that if you need a lot of medicines the cost is likely to be lower for you. You can find further information at https://www.nhsbsa.nhs.uk/help-nhs-prescription-costs/nhs-prescription-prepayment-certificate-ppc

or ask at your local pharmacy.
What medicines might I need to take?
- Nitrates (GTN)
Nitrates are medicines that help widen your heart’s blood vessels. This lets more blood, and the oxygen it carries, reach your heart.
GTN (Glyceryl Trinitrate)
This is used to relieve symptoms of angina and chest pain. For further information, see the section ‘What should I do if I have chest pain or angina?’ earlier in this information.
There are different ways in which you may take your GTN medicine:
- GTN spray
- GTN tablets
- GTN buccal tablets (tablet that dissolves between your lip and gum)
We will prescribe you those which are right for you.
How do I take GTN?
GTN Spray:
- Hold the spray upright.
- Do not shake it.
- Spray 1 or 2 puffs under your tongue and close your mouth.
- GTN works very quickly. It may make you feel lightheaded, so do sit down when you use it.
GTN tablets:
- Put 1 tablet under your tongue and let it dissolve.
- When your pain has gone, you can spit out any of the tablet which is left.
GTN buccal tablets:
- Put the tablet between your upper lip and gum.
- Leave it there to dissolve.
Points to remember
- Carry your GTN with you all the time.
- You cannot become addicted to GTN. It is not addictive and it is not a failing if you need to use it.
- Keep your GTN out of the sun and in a cool place.
- Check you have enough spray left, especially before travelling.
- You can use the spray until the expiry date on the bottle.
- GTN tablets: Throw the bottle away 8 weeks after opening. Return unused tablets to your pharmacy.
- Tip: Write the date you opened the bottle on the label.
- Keep GTN tablets in their original bottle. Do not mix them with other medicines.
What side effects might I get from taking GTN?
You may get:
- headache
- warm or red skin (this may appear differently on black or brown skin)
- dizziness
These usually last only a few minutes.
Do contact your GP if they do not settle, or if they stop you doing your normal activities.
Antiplatelets
Aspirin
As well as being used as a pain relief medicine, aspirin helps stop blood clots forming by making platelets (tiny blood cells) less sticky. This lowers your risk of having a heart attack.
- Take your aspirin once a day with food. It can upset your stomach if taken on an empty tummy.
- Tell your doctor if you get stomach pain or other symptoms. These could include bleeding, bruising, indigestion, constipation, nausea or vomiting.
- It is usually cheaper to buy aspirin from the pharmacy than to pay a prescription charge.
- Do not take other medicines that contain aspirin. For example, Anadin, Aspro, Beechams Powders, Disprin, AlkaSeltzer).
- Ask your pharmacist if you are unsure.
Clopidogrel or Ticagrelor
These medicines also help stop clots forming. Many people take one of these plus aspirin, especially after having a stent.
- Clopidogrel – take once a day
- Ticagrelor – take twice a day
- If you take Ticagrelor and become short of breath, tell your doctor straight away.
- These medicines are very important to help keep your stent clear.
- Do not stop taking them unless your heart doctor (cardiologist) says so.
- If another healthcare professional tells you to stop, ask them to speak to your cardiologist first.
- Betablockers
Beta-blocker medicines include Bisoprolol, Atenolol, Metoprolol, Carvedilol and Nebivolol
Betablockers can:
- lower blood pressure
- lower your heart beat (heart rate)
- help prevent angina
- lower your risk of another heart attack
- help control an irregular heartbeat.
How should I take my betablockers?
- Follow the instructions on the label.
- If you forget a dose, take it when you remember, then take the next dose at the usual time.
- Do not take a double dose.
- Do not stop taking betablockers suddenly. This can make angina worse or cause a heart attack.
- Do not take cold remedies such as Lemsip, Night Nurse or Benylin while on betablockers.
Be aware,
tell your doctor straight away if you become short of breath or wheezy after taking a beta-blocker.
What other side effects might I get from taking beta-blockers?
Other side effects can include:
- cold hands and feet
- pins and needles
- tiredness
- impotence
- sleep problems
- dizziness.
Do tell your GP at your next appointment if you notice any of these.
- ACE inhibitors
ACE inhibitor medicines include Ramipril, Lisinopril, Enalapril, Captopril
ACE inhibitors help:
- your heart pump more effectively
- prevent or treat heart failure
- lower the risk of another heart attack
- lower blood pressure
You will need a blood test 1 to 2 weeks after starting this medicine to check your kidneys. Please arrange this with your GP surgery or the cardiac rehab team.
Your GP may slowly increase your dose. Each time this happens, you will need another blood test.
What side effects might I get from taking ACE inhibitors?
Side effects can include:
- dry cough
- loss of taste
- headache
- rash
- dizziness
- Angiotensin 2 antagonists (ARBs)
Angiotensin 2 antagonist medicines include Losartan, Candesartan and Valsartan
These work in a similar way to ACE inhibitors but are less likely to cause a dry cough.
You will need a blood test 1 to 2 weeks after starting them to check your kidneys. Please arrange this with your GP surgery or the cardiac rehab team.
- Statins (cholesterollowering medicines)
Statin medicines include Atorvastatin, Simvastatin, Rosuvastatin, Pravastatin
Statins:
- lower cholesterol
- slow the “furring up” of the arteries
If you take Simvastatin, take it at night as this works best.
A rare side effect of statins is muscle inflammation.
Do tell your GP if you get unexpected muscle pain, tenderness, or weakness.
You will need a blood test 1 to 2 months after starting your statin to check your liver and cholesterol. Please arrange to have this with your GP surgery or the cardiac rehab team.
If you cannot tolerate a statin, ask your GP or the cardiac rehab team about other medicines that you may be able to take instead.
If you need further information about your medicines, please see the leaflet that comes with them.
Who can I contact for further information, advice or support?
- Cardiac Rehabilitation Team.
Phone: 01272 446019.
Calls are recorded on an answerphone. Our office is staffed from Monday to Friday 8am to 4.30pm. We aim to return your call within 24 hours other than at the weekend.
We are happy to speak with your family or friends on your behalf. If you would like us to do this, you must tell us that you give your consent to (agree to) this.
- Consultant Cardiac Nurse.
Phone: 01903 205111, extension 84048
Calls are recorded on an answerphone and dealt with as soon as possible.
Be aware,
neither of these contacts is an emergency line.
What do they mean? (glossary)
- Acute Coronary Syndrome (ACS)
This is a group of heart problems caused by a sudden drop in blood flow to the heart. It includes stable and unstable angina and heart attacks (also called myocardial infarctions).
- Angina
Angina is the name for symptoms caused when not enough blood reaches the heart.
Symptoms can include:
- chest pain or discomfort
- a tight or heavy feeling
- shortness of breath.
- Angiogram (Cardiac Catheterisation)
An angiogram is a test that shows exactly where the arteries around your heart are narrow or blocked.
A dye is injected into your bloodstream and X-ray pictures are taken so the doctor can see how blood flows through your coronary arteries.
- Angioplasty
This is a treatment used to open up a blocked or narrowed artery.
It helps improve blood flow to your heart muscle.
- Atherosclerosis
This means a buildup of fatty substances inside the artery wall.
The buildup (called plaque) includes:
- fat
- cholesterol
- waste products from cells
- calcium
- fibrin (a bloodclotting protein)
Over time this narrows the arteries, making it harder for blood to pass through.
- Cardiac Enzymes (Troponin)
Troponin is a substance in the blood that helps doctors check if the heart muscle has been damaged or is not getting enough blood.
If blood supply is reduced, troponin levels rise, which helps doctors decide if someone has had a heart attack.
- Cholesterol
Cholesterol is a fatty, waxy substance made mostly by the body.
The liver also makes cholesterol from foods high in saturated fat (such as meat, dairy products and processed foods).
- Coronary Artery
A coronary artery is a blood vessel that supplies the heart muscle with oxygen and nutrients in the blood.
- Coronary Heart Disease (CHD)
CHD happens when fatty deposits build up inside the coronary arteries (atherosclerosis).
This can narrow or block the arteries and reduce blood flow to the heart.
- Diabetes Mellitus (Diabetes)
Diabetes is a condition where the body cannot control blood sugar levels properly.
It may be treated with:
- changes to your diet
- medicines, tablets or insulin injections
- Echocardiogram (Echo)
An echocardiogram is an ultrasound scan of the heart.
It shows the shape, size, structure and movement of the heart and how well it is working.
- Electrocardiograph (ECG)
An ECG is a test that records the electrical activity of the heart.
It shows:
- how fast the heart is beating
- whether the rhythm is regular
- whether the heart is getting enough blood
- Glyceryl Trinitrate (GTN)
GTN is a medicine used to relieve angina symptoms. It works by widening the arteries so more blood can flow through. It may be given as a spray or tablet.
- Myocardial Infarction (MI or
- Heart Attack)
A myocardial infarction (heart attack) happens when the blood supply to part of the heart is very limited or completely blocked.
This can cause permanent damage to the heart muscle.
It needs emergency treatment.
- Myocardial Perfusion Scan
This is a test that uses a small amount of radioactive material to show how well blood reaches the heart muscle.
Pictures are taken:
- at rest, after the radioactive material is injected
- under stress, when a drug is used to make the heart work harder (as if you were exercising)
- PCI (Percutaneous Coronary Intervention)
PCI is another name for angioplasty.
It is the procedure used to open up narrowed heart arteries.
- Stent
A stent is a small wiremesh tube used to keep a coronary artery open after an angioplasty.
It acts like a scaffold inside the artery.
- Plaque
Plaque is the fatty deposit that builds up inside artery walls during atherosclerosis.
It can narrow the arteries and reduce blood flow.
- Risk Factor
A risk factor for coronary heart disease is anything that makes it more likely that a person will develop coronary heart disease.
Useful contacts phone numbers:
Age UK – Information and Advice
0800 678 1602
Alcoholics Anonymous
0800 9177650
British Heart Foundation (BHF)
0808 802 1234
Cardiac Rehab Worthing and Southlands
01273 446019
Cardiac Rehab Chichester and Bognor
01243 831829
Cardiac Rehab Royal Sussex County Hospital
01273 696955
Ext. 64009
Citizens Advice Bureau
0800 144 8848
Diabetes help-line line Worthing Hospital
01903 205111
Ext. 85543
DVLA (medical enquiries)
0300 790 6806
Heart Failure Nurse helpline
01903 205111
Ext. 84595
Universal Credit helpline
0800 328 5644
NHS Direct
111
NHS Smoking helpline
0300 123 1044
Smoke Free West Sussex (help with stopping smoking)
0330 222 7980
Patient Advice & Liaison Service (PALS)
01903 285032
Samaritans – National
116 123
Worthing and Southlands Hospital (Switchboard)
01903 205111
Which websites might I find useful?
- The Cardiac Rehab team have their own website with information on the service we provide
- The British Heart Foundation have information on all aspects of heart conditions
- Heart UK
- Cardiomyopathy UK Helpline
- Pumping Marvellous
- DVLA (for any queries relating to driving and driver licensing)
- Cardiac Rehab Support
This is a local registered charity formed from some ex-patients who aim to provide ongoing support for cardiac patients and their carers.
Use the space (see PDF at the top of this leaflet) to write any notes or questions that you have. We are keen to know if this document gives you the information you need in a way that is easy to understand. Please tell us if you think we can improve it by emailing our Carer and Patient Information Group [email protected]
This leaflet is intended for patients receiving care in Worthing and Southlands Hospital.
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Today’s research is tomorrow’s treatments. That’s why UHSx is proud to be a research-active Trust. Find out how you can get involved.
Visit our website www.uhsussex.nhs.uk/research-and-innovation/information-for-patients-and-public or scan the QR code: