Download and print as a PDF (2MB pdf)
On this page
- What is a gastroscopy?
- Who will be performing my procedure?
- Are there any significant risks?
- What are the benefits?
- Are there any alternatives?
- How do I prepare for my examination?
- What should I bring with me to the unit?
- Can I park at the hospital?
- What happens when I arrive in reception?
- What happens after my examination?
- Frequently asked questions:
- Your comments and suggestions
- Who can I contact for further information and advice?
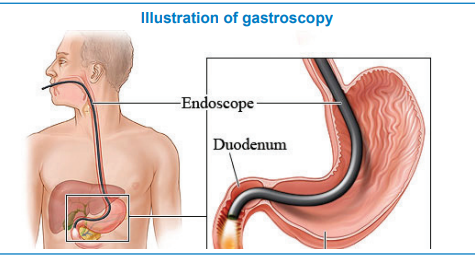
What is a gastroscopy?
This is a simple examination which enables the endoscopist to view the inside of your oesophagus (gullet), stomach and duodenum (small bowel). A tiny camera on a flexible tube will be carefully passed into your mouth and down your oesophagus.
It is not a painful examination and does not interfere with your breathing. However, some people may find it uncomfortable, so we can give you a sedative or throat spray to anaesthetise the back of your throat. The sedative will make you feel relaxed and drowsy. This will be explained in more detail by the nurse who will assess you. If you have any questions or concerns, please don’t hesitate to ask.
Who will be performing my procedure?
The procedure will be performed by specially trained healthcare professionals. Occasionally, supervised doctors or nurses in training will be performing the procedure. Brighton and Sussex University Hospital is attached to the Brighton and Sussex Medical School and as such medical students may also be in attendance. If you do not want students present, please inform the nursing staff on your arrival.
Are there any significant risks?
These telescopic examinations are very safe but some risks are associated with the procedure:
These include a reaction to the sedative which can affect 1:2500 people. This may affect your breathing or blood pressure, both of which are closely monitored during any procedure. A tear or perforation in the lining of the bowel can occur in any telescopic test. The national figures for this are 1:1500.
If this does occur you will need to be admitted to hospital and may require an operation to repair the tear.
Minor bleeding is common if biopsies or pieces of tissue (polyps) are removed but this bleeding usually stops spontaneously. More significant bleeding can occur in 1:1000 procedures and may require admission to hospital and a blood transfusion. Specialist equipment and training reduce all these risks considerably. The figures quoted here are national averages and for this Trust are much lower. There is also a risk of small lesions being missed. This is currently quoted as approximately 5%.
Please speak to the doctor or nurse performing your procedure if you have any concerns.
What are the benefits?
This procedure allows direct visualisation of your gullet, stomach and small bowel. It also enables biopsies to be taken.
Are there any alternatives?
The only alternative is a Barium Swallow. This is an x-ray test which requires you to drink a special liquid that enables the stomach to be visualised. It does not allow tissue to be sampled or removed.
How do I prepare for my examination?
- Have nothing to eat for six hours before the examination. Do not drink any milk products after this time.
- Have nothing to drink for two hours before the examination.
- If you are able to, without too much discomfort, please stop taking the following tablets two weeks before your appointment:
- Omeprazole (Losec)
- Lansoprazole (Zoton)
- Pantoprazole (Protium)
- Rabeprazole (Pariet)
- Esomeprazole (Nexium)
Be advised
If you have been told to stay on your medication or if you have previously had an ulcer, oesophageal varices or Barrett’s Oesophagus please do not stop taking them
- If you are a diabetic on medication (insulin or tablets) and need advice, please contact the health professional who looks after you regarding your diabetes. If you do not have a health professional who looks after you regarding your diabetes, please call the hospital on 01273 696955 extension 64205 and speak to one of the Diabetes Nurse Specialists.
- Following arrival you will be seen by the admitting nurse. Once the admission process has been completed you may be offered a small pre-procedure drink. This drink is an oral preparation to help clear the oesophagus and stomach of any mucus, saliva or remaining food debris.
- If you have ever been informed that you are at risk from CJD or vCJD for public health purposes, please call us on 01273 696955, extension 64570 (Royal Sussex County Hospital) or 01444 441 881, extension 68187 (PRH).
- It is very important that you follow all the instructions carefully, or your examination may need to be postponed.
What should I bring with me to the unit?
- If you are having sedation for your procedure you will need someone to act as an escort and stay with you for the remainder of the day and overnight. Your escort must come up to the unit to collect you. We cannot take you down to meet them
- A list of all your medication
- Your reading glasses
- Wear loose and comfortable clothing
- Music if you find it relaxing
- Do not bring any valuables with you
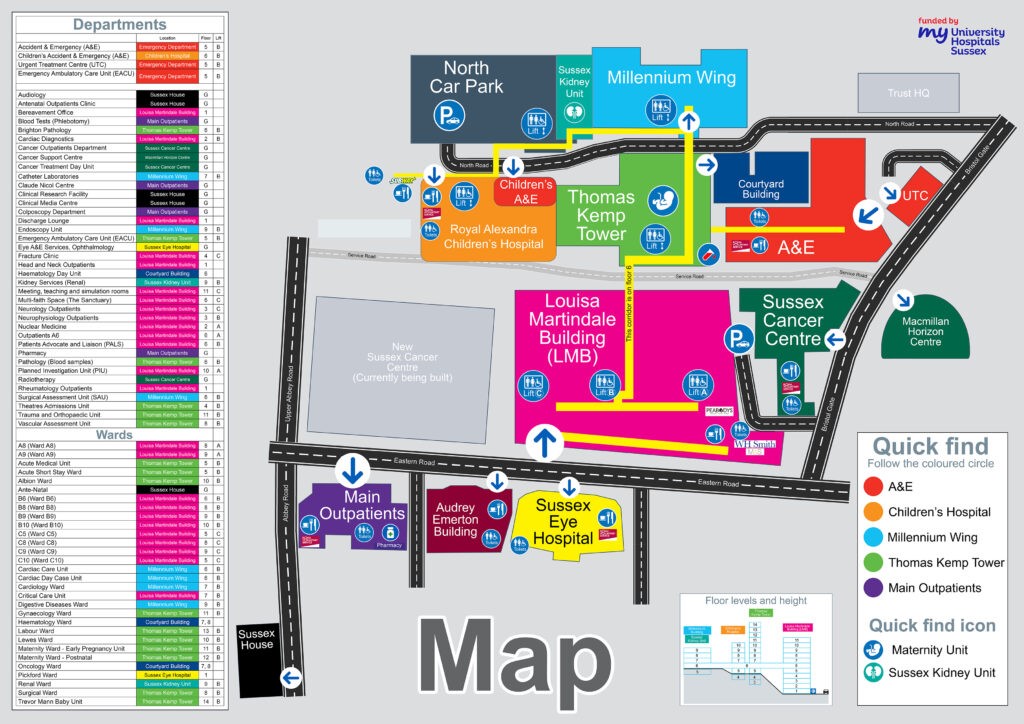
Can I park at the hospital?
Parking space at the Royal Sussex County Hospital is very limited, so please set off in plenty of time for your appointment and be prepared to wait in the car park queue. Alternatively, your escort may drop you off at the Millenium Wing and then return to the unit to collect you later.
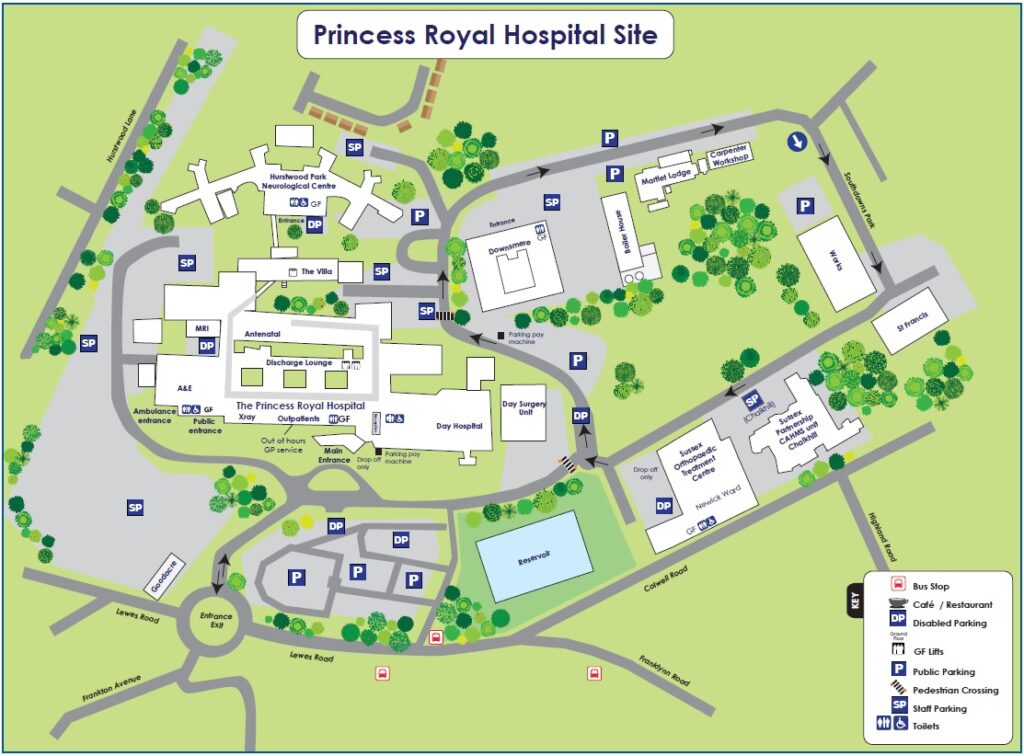
There is ample parking at the Princess Royal Hospital.
If you have sedation for your procedure and intend to go home by taxi, you will need a responsible adult to accompany you, as taxi companies will not accept responsibility for you travelling alone. Although you may use public transport to come to hospital, we strongly advise you not to travel home by bus or train, following sedation.
It is very important that you follow all the instructions carefully, or your examination may need to be postponed.
What happens when I arrive in reception?
Please report to the desk. Our receptionist will check your details and ask you to take a seat in the waiting room. You will then be called through by a nurse or health care assistant, who will explain the examination to you and ask you some questions about your medical history. Prior to your examination we may give you something to drink to ensure your stomach is empty. If you are having sedation, please ensure that you have your escort’s contact details with you so that we can call them when you are ready to be collected. You will be asked to sign a consent form before the examination. Please see a copy of the form at the back of this booklet. If you have any questions or if there is anything at all that you don’t understand, please ask.
What happens after my examination?
If you have had sedation for your procedure you will have time to rest and will be offered a drink and a biscuit. You will need to rest for the remainder of the day and refrain from smoking and drinking alcohol. If you have a gluten allergy please bring something to eat.
If you had a sedative, you must not drive, sign legal documents or operate machinery for 24 hours. You should have a responsible adult to act as your escort and stay with you for the remainder of the day and overnight.
An explanation of the examination findings will be given to you by a nurse or doctor. You may need to make an appointment to see your GP, who will receive a report of the examination within a week.
Frequently asked questions:
Will it hurt?
Endoscopic examinations and procedures can be uncomfortable, so we have a variety of interventions at our disposal to make it more comfortable for you. We can give you a local anaesthetic or sedation for gastroscopy. After a gastroscopy you may suffer from a sore throat and bloating. These effects should disappear after a few days but you will be given written aftercare advice when you go home, which tells you what to do if your symptoms do not settle.
How long will it take?
Examination and procedure times vary. A simple diagnostic examination should take between five and ten minutes but a more complicated examination, involving endoscopic treatment, such as removal of polyps, can take anything from 30 minutes to 90 minutes, or longer. If your examination involves having treatment, your recovery time will also be slightly longer. This is why you should be prepared to be in the unit for possibly 3 to 4 hours.
When will I get my results?
Results from biopsies taken, or polyps which have been removed, may take up to eight weeks to come back from the laboratory. The findings are reviewed by your consultant, who will then arrange follow up. This could be a clinic appointment to discuss your results or it could be a letter explaining your results. Please do not phone our recovery area during this time: we are unable to give any biopsy results over the telephone. If you have not heard anything after eight weeks, and you are worried, please contact your GP, who will be informed of your results.
What do I do if I need to cancel or change my appointment?
If you need to cancel or change your appointment please call us on 0300 303 8517.
Your comments and suggestions
If you have any concerns about your treatment or care, please bring them to our attention. We will do our best to help.
If you feel you would like some support with raising your concerns, the Patient’s Advocate is available to speak on your behalf.
You can contact the Patient’s Advocate by telephone between 10am and 4pm on: 01444 441881, extension 65909 (Princess Royal Hospital) or 01273 696955, extension 64029 or 64588 (Royal Sussex County Hospital), or by email at [email protected] for either site.
We always welcome new ideas and suggestions. Please let us know if you feel there are ways in which we could improve our service.
Who can I contact for further information and advice?
Thank you for taking the time to read this information: if there is anything at all that you don’t understand, or you have any questions, please ask a nurse at the unit, or call us on 01273 696955, extension 64570 for the Royal Sussex County Hospital and 01444 441881, extension 68187 for the Princess Royal Hospital.
At the end of the leaflet is an example of the form ‘Patient agreement to investigation or treatment’. Please print off the PDF version to obtain the example form.
This information is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information here is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.