Download and print as a PDF (382kB pdf)
On this page
What is happening?
The doctors and nurses looking after you think that your symptoms may be caused by a blood clot blocking blood supply to the brain. If left untreated this may result in a disabling stroke. A stroke can potentially cause limb weakness, speech difficulty, visual changes and other complications. Quick treatment is needed to restore the blood supply to the affected area of the brain.
How can this be treated?
For some patients the first line of treatment is a drug called Alteplase. This is a clot busting drug. The administration of this drug is known as ‘thrombolysis’. The aim of thrombolysis is to dissolve the clot and get the blood flowing back to the affected area of the brain.
Thrombolysis must be given within 4.5 hours from the start of symptoms to stand a good chance of being effective. In some people, Alteplase cannot be given if there are significant bleeding risks. Some people may be suitable for an additional procedure to remove the clot mechanically. This is called a thrombectomy.
How is a thrombectomy performed?
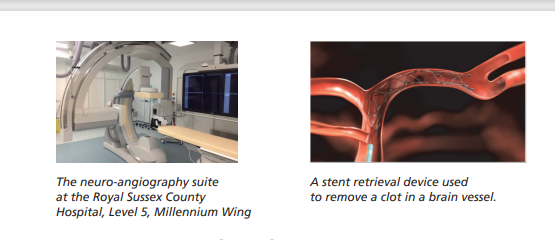
Thrombectomies are performed by a specialist team at the Royal Sussex County Hospital, and involve a thin plastic tube (catheter) being inserted, usually through an artery in the groin. The catheter is then moved, through the blood vessels in your body, to the blocked blood vessel in your brain. A contrast agent (dye) is injected into the catheter and x-ray is used to look at the blood vessels (an angiogram). If the artery is still blocked, the doctor will try to remove the clot, either by suction or by pulling it out with a special device called a stent retriever.
A doctor called an interventional neuro radiologist will perform the thrombectomy. A radiographer will operate the x-ray machinery. Nurses will be available to assist during the procedure and to monitor and reassure you. Most procedures are performed awake using local anaesthetic to numb the groin. Sedation may be used if you become restless, which can occur following a stroke. Sedation helps to reduce the risks to restless patients. You may also feel some discomfort or pain during the procedure, and if this occurs pain relief can be given.
The procedure may be abandoned if it becomes too unsafe due to you being too unwell or too restless to tolerate it. In some cases an emergency general anaesthetic may be required. The procedure can take up to an hour to complete, though in some cases this may be much quicker or slightly longer. Occasionally, it may not be technically possible to retrieve the clot. This can be due to damaged or blocked blood vessels.
What are the benefits of thrombectomy?
Removing the blood clot from the blocked vessel leads to better outcomes including greater independence and mobility. 8 out of every 20 patients that undergo thrombectomy will recover with less disability. Not every patient will benefit however (because some damage to the brain has already happened). Severe complications from the procedure happen infrequently (in less than 1 in 20 patients) and the chances of a bad outcome do not increase as a result of this procedure.
What are the risks of thrombectomy?
• Small risk of allergic reaction from the contrast agent (the ‘dye’ we use to see the arteries and veins on x-ray pictures). In rare cases it can permanently harm the function of the kidneys.
• Bruising or swelling at the groin where the catheter is inserted. Only in very rare cases is this severe enough to require surgery to repair the groin artery.
• The angiogram can cause stroke (1% of patients).
• Bleeding in the brain can occur. This can be serious (less than 4% of patients) and potentially fatal.
• There is a very small risk of infection.
Asking for your consent
Before we can go ahead with treatment, by law we must explain the risks and benefits to you, discuss alternative treatment options, and then seek your consent.
If you are too unwell to be able to give informed consent the doctors will proceed in your best interests. However every effort will be made to speak with your next of kin or anyone who holds lasting power of attorney for health and welfare. This discussion will cover your known wishes and beliefs, and whether treatment is likely to be in your best interests.
What to expect after the thrombectomy
After the thrombetomy procedure has finished you will be taken to the stroke ward and cared for there by the stroke team (doctors, nurses and the different therapists). You will be on bed rest for a couple of hours to allow the puncture site to heal, as well as your vital observations being checked regularly.
You can expect to experience some pain from the groin. This can be managed on the ward with analgesia.
If you have been transferred from another hospital we would usually aim to repatriate you back to your local stroke centre after 24 hours if your condition is stable. This can take longer however, and is partly dependent on bed availability. Whilst you are still in Brighton you will continue to receive all the usual care provided to someone after a stroke.
Useful information
Stroke Association
Helpline: 0303 3033 100
This website enables you to find stroke support groups and information in your local area.
The stroke wards at The Royal Sussex County are Donald Hall and Solomon wards. They are located on the third floor of the Barry Building. The main contact for the stroke ward is Mark Holmes (ward manager); however, if you phone the ward there will usually be a member of the stroke team available to speak to.
If, following discharge from Brighton or transfer to another hospital you wish to speak to someone regarding your procedure please also contact the ward and a member of the team will usually be available to speak with you.
01273 0696955 Ext. 64006
Additional services
Patient Advice and Liaison Service (PALS)
PALS can offer you on-the-spot advice and information when you have comments or concerns about our services or the care you have received.
Contact details as follows:
Royal Sussex County Hospital:
01273 664511 or 01273 664973
[email protected]
PALS, Royal Sussex County Hospital, Eastern Road, Brighton, BN2 5BE
This leaflet is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.