Download and print as a PDF (429kB pdf)
On this page
- Introduction
- How can you help us before you come in for your surgery?
- What will happen in the Pre-Assessment Clinic?
- What about my usual medicines?
- What can I eat and drink before my operation?
- When do I have my pre-operation medication?
- What about infection control?
- What can I expect after my caesarean section?
- Why are exercises an important part of my recovery?
- What should I do if I have concerns after I leave hospital?
- Will I need a follow up appointment?
- What should I bring into hospital?
- Visiting times
- What is my Daily Diary?
- References and useful links
Introduction
The aim of the Enhanced Recovery Programme (ERP) is to get you back to full health as quickly as possible after your caesarean. Research indicates that after surgery, the earlier you get out of bed and start eating and drinking the better. This will speed your recovery making it less likely that complications will develop. For example, the benefits of getting up and about are:
- Returning to eating and drinking much sooner
- Reduced risk of hospital acquired infection
- Less tiredness
- Reduced risk of developing blood clots
To achieve this, however, we need you to be a partner with us so that we can work together to speed your recovery. This article will increase your understanding of the programme and ensure you play an active role in the preparation for your operation and your recovery.
Before you come into hospital your obstetrician/midwife will see you and explain the programme to you, where you will be given the opportunity to ask questions.
Below is a picture of your female anatomy while pregnant. Your obstetrician will explain your operation to you.
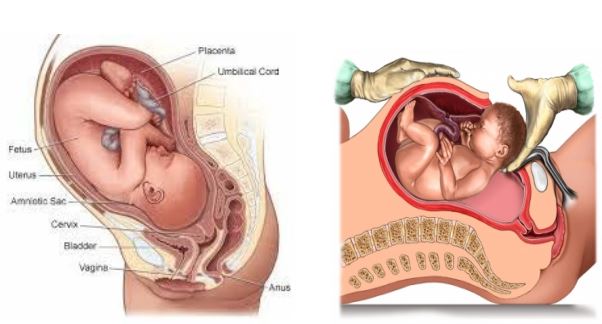
How can you help us before you come in for your surgery?
If you optimise your health in the weeks before your operation then you will recover more quickly and have fewer complications.
Try to eat as healthily as possible and you may consider taking a multivitamin every day to make sure you have a good level of essential nutrients. Do not diet in the weeks before an operation but also avoid putting on a lot of weight. Ensure adequate exercise and walk whenever you can. If you are a smoker it is advisable for you to stop. You may wish to speak to your Community Midwife, GP or contact the National Stop Smoking helpline on 0800 022 4332.
Also, think about how you can cope in the weeks after surgery when you are convalescing. Can you arrange help from family or friends? If you think that you will have problems at home after your operation then seek help early so a suitable solution can be found before your operation.
Make sure that you raise any concerns that you have in the preassessment clinic. If you look after your health in the weeks before your operation then you will recover quicker and have fewer complications.
What will happen in the Pre-Assessment Clinic?
The day before your admission date you will be seen in the pre-assessment clinic. The clinic is run by experienced midwives and maternity care assistants, where you will be given your pre-operation medication; you will also need to have blood taken in the phlebotomy department.
You will also have a thromboprophylaxis risk assessment to prevent Deep Vein Thrombosis. A copy of the leaflet Prevent Deep Vein Thrombosis (DVT) whilst in hospital, will be given to you.
What about my usual medicines?
Please bring into hospital any medication that you usually take on prescription in their original boxes. The midwife in pre-assessment will tell you which of these should be taken before and on the day of your surgery.
What can I eat and drink before my operation?
You can have 500mls of Lucozade sport two hours prior to you admission or until 7am and then you will need to fast (be Nil by Mouth).
If you are a type one diabetic or gestational diabetic on insulin or diet controlled you can have clear fluids only.
| Admission Time | No food from: | Isotonic Lucozade sport | Clear fluids until: | Diabetics Clear fluids until: |
|---|---|---|---|---|
| 8:00am | 22:00pm | 6:00am | sip till send into theatre | over night sip till send into theatre |
| 11:00am | 3:00am | 6:00am | sip till send into theatre | over night sip till send into theatre |
When do I have my pre-operation medication?
If my operation is in the morning:
10pm and 6am.
If my operation is in the afternoon:
10pm and 10am
What about infection control?
Hand hygiene is the best way to prevent germs spreading. It may feel awkward to question staff when someone is looking after you, but you are entitled to ask/remind health care staff to wash their hands.
To help reduce the risk of getting an infection in hospital, please read the following advice.
- Keep your hands and body clean
- Always wash your hands before and after using the toilet
- Always wash your hands or use a moist wipe before you eat your meal
- If a member of staff needs to examine you or perform a procedure, do not be afraid to ask if they have first washed their hands or used a hygienic hand rub. Staff should gloves for procedures such as taking blood, undertaking dressings etc.
- Keep your locker and bedside table tidy and free from clutter and ensure none of your possessions are on the floor. This will make it easier for staff to clean properly
- Ask your visitors to use the hand gel provided on entering and leaving the ward
- Please remember flowers are not permitted throughout the hospital.
What can I expect after my caesarean section?
After your caesarean section you will be transferred to a delivery room for recovery, this could be a two bedded bay. Where you will stay for the minimum of two hours or until your observations are stable. During this period of recovery you will be offered a light snack and a drink and your cannula will be removed and help will be given for feeding support. Your assigned midwife will then transfer you to the postnatal ward. You will be given a leaflet specific to your surgery that will tell you what to expect postoperatively and will advice you on ‘dos and don’ts’.
Why are exercises an important part of my recovery?
The quicker you begin to start moving around, the quicker you may leave hospital. Your recovery starts immediately after your surgery and you will be encouraged to mobilize and your catheter will removed after six hours to reduce the risk of infection.
These five top tips aim to provide a visual prompt to aid mobilisation and exercise in the early days.
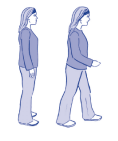
How should I stand?
- Stand straight
- Gently pull your lower stomach muscles in before you start walking
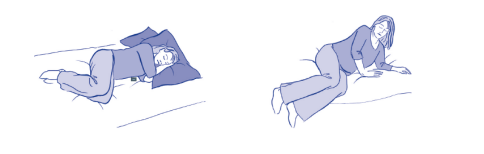
How should I get in and out of bed?
From lying on your side as above, push through your arms to lift your head and trunk up, and at the same time allow your feet to lower over the side of the bed for a few moments, and then stand up by leaning forwards and pushing up with your hands and legs. Try not to stoop, stand tall
What should I do if I need to cough?
Lean forwards, and cough using a pillow or towel for support.
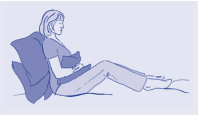
How should I sit?
- Sit well back in the chair
- Make sure your feet touch the floor
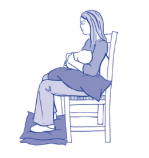
What is the best position to help me empty my bowels?
- Keep your knees apart and higher than your hips
- Lean forwards
- Let your stomach muscles relax and bulge outwards making your waist widen

Can I start exercising my pelvic floor muscles?
- Yes, as long as you feel comfortable. It is important to carry on exercising your pelvic floor muscles after delivery of your baby/babies
- Remember, to imagine you are trying to stop yourself passing urine and at the same time trying to stop yourself from passing wind
- You can practice short and long squeezes
- Don’t hold your breath
You will find more detailed information in the post-natal booklet when you leave hospital.
What should I do if I have concerns after I leave hospital?
Complications do not happen very often. However it is important that you know what to look out for. If you are worried during the first four weeks after surgery then please contact us.
Abdominal pain
If you have severe pain lasting for more than two hours or have a fever and feel generally unwell please contact us and we will advice you.
Vaginal discharge, or bleeding
You can expect to have some vaginal discharge, or bleeding for four to six weeks after surgery. This is like a light period and is red or brown in colour. Sanitary towels should be used, not tampons, to reduce the risk of infection. If you experience any heavy bleeding and you’re concerned please contact us.
Your wound
It is not unusual for your wounds to be slightly red and uncomfortable during the first one or two weeks. Please let us know by telephone if your wounds become inflamed, painful or swollen or start to discharge fluid.
Your bowels
Your bowel habits may change temporarily. Your motions may become constipated or may become loose. Make sure you eat regular meals three or more times a day, replace any fluid lost and take regular walks. In most patients their bowels settle down a few weeks after surgery.
Passing urine
Sometimes after a caesarean section you may experience a feeling that your bladder is not emptying fully. This usually improves with time. If it does not improve or you have excessive stinging when passing urine, you must make an appointment to see your GP. Take a sample of urine with you or be prepared to give a sample if asked to at your appointment
Will I need a follow up appointment?
Your midwife will come and see you regularly at home and check your scar is healing well. If you are worried about anything, please contact your community midwife or labour ward at the hospital.
You will need to have a check at six weeks with your GP. If you wish to discuss any aspect of your caesarean or future pregnancies, please talk to your midwife or GP. Many women who have had a caesarean section go on to have a vaginal birth next time. You can start having sex again whenever you feel ready but remember that you will need to use contraception as you can get pregnant again straight after having a baby. We do not advise that you get pregnant within three months of a caesarean.
What should I bring into hospital?
Always bring this booklet with you as it contains your patient diary and all the information you need.
We suggest you bring in
- Toilet bag with wash things
- Sanitary towels
- Loose-fitting night clothes
- Baby clothes
- Cotton wool
- Nappies
- Dressing gown and slippers (Comfortable footwear)
When you come to stay in hospital for your operation, do not bring in anything of potential value e.g. jewellery, credit cards etc. Please keep your property to a minimum, as there is limited space in your locker.
Please arrange for friends/relatives to take bulky items such as bags/suitcases home as soon as possible for access to clean around your bed area and storage issues. Please do not send your outdoor clothes home as you will need them the morning of your discharge.
Visiting times
- Royal Sussex County Hospital, Eastern Road, Brighton: to be arranged
- Princess Royal Hospital, Lewes Road, Haywards Heath: to be arranged
Only two visitors at a time on the postnatal wards.
What is my Daily Diary?
On the PDF version of this information, available to download at the top of this page, we have written a diary that we want you to complete on the first few days after your operation. This will help guide you and hopefully get you more involved with striving to ensure a good recovery.
Each day please complete your personal activity plan. If you didn’t achieve an activity there is space for you to document why not and also for other thoughts etc that you may wish to write down.
References and useful links
- NHS Improvement (2011) Enhanced Recovery
- Department of Health (2010) Enhanced Recovery
- Pelvic, Obstetric and Gynaecological Physiotherapy (POGP)
This leaflet is intended for patients receiving care in Brighton and Hayward’s Heath.
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.
Today’s research is tomorrow’s treatments. That’s why UHSx is proud to be a research-active Trust. Find out how you can get involved.
Visit our website www.uhsussex.nhs.uk/research-and-innovation/information-for-patients-and-public or scan the QR code: