Download and print as a PDF (4MB pdf)
On this page
Welcome
Congratulations on your pregnancy!
This guide provides information to help you prepare for feeding and caring for your baby or babies.
Talk with your midwife and have open conversations about getting ready to meet your baby, and come along to our antenatal classes to find out more. We will support you every step of the way and will let you know about local and national support.
Scan here to visit our UHSussex Infant feeding pages with links to our Padlet for lots more
information and great videos to help you get off to the best possible start.

Flying Start: Feeding and Nurturing your Baby (padlet.com)
At University Hospitals Sussex we celebrate inclusivity and diversity and support all parents to make informed decisions around infant feeding. This document should be taken to include people who do not identify as women but are pregnant or have given birth. Please speak with us about your infant feeding choices and language preferences.
Brain development
Comforting your baby helps them manage their emotions and helps their brain development.
Babies brains grow and develop very quickly during the first 1,001 days, the time between pregnancy and their second birthday. The way they are fed and cared for shapes their brains for life.
Building your babies brain can start in pregnancy. Did you know that by 19-21 weeks your baby can respond to music and by 33-35 weeks your baby has a fully developed brain and nervous system.
You can help your baby’s brain development by:
- Taking time to relax: stress in pregnancy has been shown to increase the chances of your child having mental health issues when a teenager. Try mindfulness or breathing exercises.
- Talking to your baby.
- Stroking your bump.
- Playing music.
- Reading to your baby.
- Feeling your baby’s kicks.
These activities can involve other close family members too: for example, the co-parent and older siblings.
Ways to connect and bond with your baby after they have been born:
- Hold and cuddle them.
- Smile and talk to them.
- Read to them.
- Sing to them.
- Wear them in a sling or baby carrier.
Myth buster!
It is a myth that babies become spoilt and demanding if they are given too much attention – in fact, quite the opposite is true! After they have been born, babies have a strong need to be close to their parents, as this helps them feel secure and loved. When babies feel secure, they release a hormone called oxytocin. This acts as a fertiliser for their growing brain, helping them to be happy babies and more confident children and adults.
Keeping them close also helps you to recognise the signals your baby makes when they need you, such as if they are hungry or need a cuddle.
Be advised
Human milk is species-specific and is the perfect nutrition for brain development. It is high in carbohydrates (perfect food for rapid brain growth) and contains many properties that cannot be replicated in formula milk.
Love
Your baby needs lots of love and cuddles.
Oxytocin is the love hormone that is released when you and your baby are close and it makes babies happy. Skin to skin is a great way to start, and do it as often as you like, no matter how you feed your baby.
Skin to skin contact
Skin to skin means holding your baby naked or dressed only in a nappy against your skin. Having skin to skin contact with your baby will keep them warm and calm and steady their breathing.
After your baby is born, hold them against your skin as soon as possible, and for as long as you want. It is beneficial for your baby to remain skin to skin until after their first feed or for a minimum of at least an hour. This is sometimes known as The Golden Hour. Ideally, much of the first few days will be spent cuddled up skin to skin with your baby.
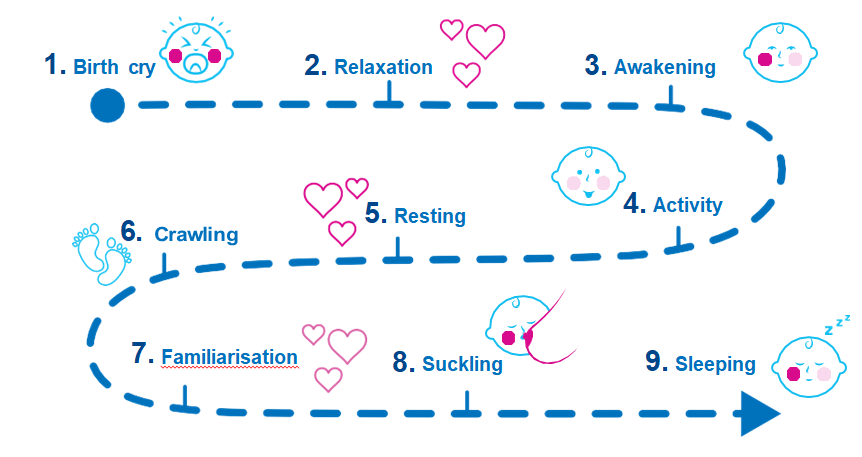
Be advised
Protect the first 60-90 minutes so your baby can go through the 9 instinctive stages.
There is strong scientific evidence that uninterrupted skin to skin supports not only the first feed, but subsequent breast feeds too.
The hormones released during this special time initiates strong instinctive behaviour both in the mother/birth parent and baby. Give yourself and your baby time to connect and for your baby to find and attach to the breast.
If you choose to bottle feed your baby, skin-to-skin is important for you too. Feed your baby whilst holding in skin-to-skin contact and looking into their eyes. This will release the love hormone oxytocin and will help you bond.
There will be plenty of time to talk to family, take photos and share your beautiful new addition with the world.
Please take advantage of the precious first hours after birth to bond and connect with your baby, with uninterrupted skin to skin cuddles.
Be advised
If your baby is born premature, please ask your neonatal team about kangaroo care.
Great start to feeding
Preparing for feeding your new baby.
Talk with your midwife and have open conversations about getting ready to meet your baby, and come along to our antenatal classes to find out more. We will support you every step of the way and will let you know about the local and national support.
Expressing colostrum while pregnant
The first milk you produce during pregnancy and in the first few days after birth is called colostrum. It’s thick and usually a golden yellow colour. It’s a very concentrated food, so you will only produce a small amount. A little goes a long way in your baby’s tiny tummy!
Colostrum is perfectly made for your baby.
Colostrum helps boost and support your baby’s immune system.
Colostrum helps protect against jaundice by acting as a laxative.
Colostrum is rich in vitamins and minerals, and full of protein.
Regardless of how you are planning on feeding your baby, giving your baby colostrum is the best way to support your baby to adjust to life outside the womb.
Learning how to collect colostrum before your baby is born will enable you to:
- Get breast feeding off to the best start.
- Feel more confident with hand expressing after your baby is born.
- Avoid or reduce the risk associated with using formula milk if supplementation is required.
- Help stimulate your baby to attach to your to the breast.
- Relieve engorgement or blocked ducts.
- Prevent or treat low blood sugar (hypoglycaemic) episodes in at risk babies – breast milk achieves and maintains blood sugars more efficiently than manufactured milks.
When can you start collecting colostrum?
From 36 weeks of pregnancy. Please ask your midwife for 1ml oral syringes as the time approaches.
How often?
Once a day is sufficient to practice the technique, but you can do more.
Remember: When you first start to express, it is common to only get a few drops of milk. The more you practice, the easier it gets. Try expressing at different times of day to see what works better for you.
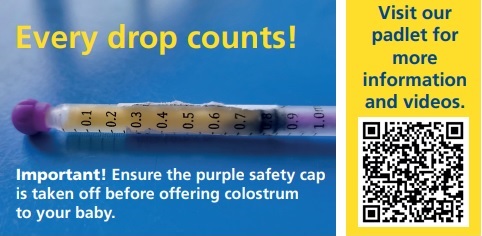
How to hand express
- Applying some warmth to the breast before expressing may help (hot flannels or a shower). Take your time, relax and think about your baby.
- Wash your hands before starting and then try some gentle breast massage and nipple rolling.
- Collect with 1ml oral syringes or a sterile container.
- Cup the breast using your thumb and index finger in a ‘C’ shape, about 2-3cms away from the base of the nipple. The location of your milk ducts varies in each woman, so your fingers may need to be further from/closer to the nipple.
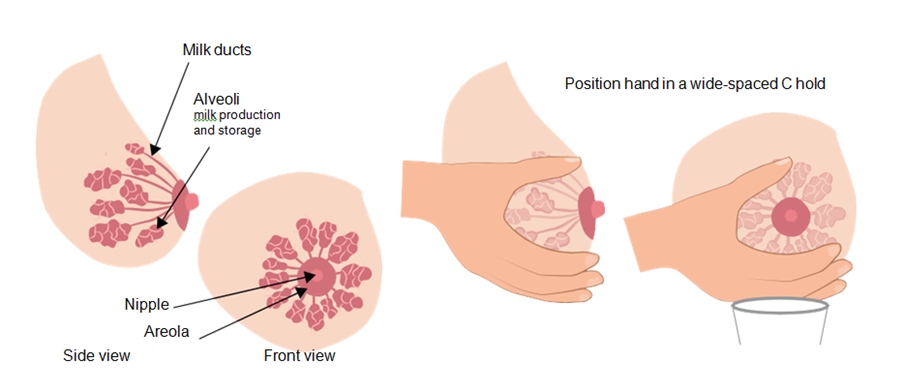
- Compress your finger and thumb together, this should not hurt.
- Relax and repeat the action, developing a rhythm.
- Avoid sliding or dragging the skin, or pinching the nipple.
- After a few minutes or after the flow of milk has stopped, rotate finger and thumb around to another position and express again.
- Move to the other breast when rotation fails to bring a new flow of milk.
Learning to breast feed
Breastfeeding is something that you and your baby will learn together.
Tips for positioning your baby at the breast:
- C: Close to mother/nursing parent
- H: Head free – no fingers or hand on your baby’s head
- I: In line – your baby’s head and body should be in a straight line
- N: Baby’s nose opposite nipple
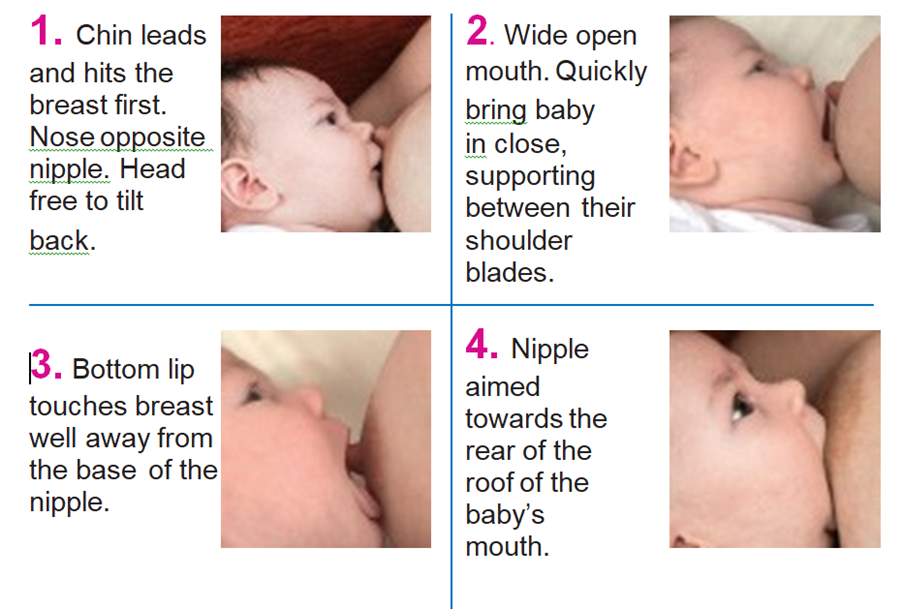
Breastfeeding positions
There are several different positions you can try until you find the one that works best for you and your baby. Get yourself comfortable and have snacks and drinks nearby. Remember to bring your baby to you, not the other way round!
Laid-back breastfeeding/biological nurturing
It is helpful to use your baby’s natural reflexes to encourage them to latch, which is why the laid-back breastfeeding position (also known as biological nurturing) can work so well. This position is also really comfortable, and there is growing evidence that it helps baby to feed more effectively.
- Lean back on a chair or bed, with your back, shoulders and arms supported by pillows.
- Place your baby in the middle of your chest (skin to skin if possible) so their tummy is against your body.
- Support your baby with your arms, and allow their feet to rest on your legs or the chair/bed.
- Once your baby feels stable, their natural instincts will prompt them to bob their head in search of the breast.
- You may need to gently guide them towards the breast if they struggle to find it themselves. You can support their body using your hands on their thigh or bottom.
- Gravity will help your baby to latch deeply and stay latched on.
- If you feel pain (beyond a few seconds) detach baby gently by putting your finger in the corner of baby’s mouth, and then allow baby to try to latch again.
- Relax and enjoy the feed!

Cross cradle position
Hold your baby really closely, with their head and body in a straight line.
You can support your baby’s back with your forearm. Hold your baby between their shoulder blades, ensuring your baby’s head is free from your hand or any fingers. This will allow them to tilt their head back. This is a really important point!
Bring your baby to your breast, so they are leading with their chin, with their nose exactly opposite your nipple. Their top lip will brush past your nipple. When they open their mouth wide, bring them swiftly to your breast. Your nipple should fit comfortably in the roof of your baby’s mouth. Once your baby is feeding you can bring your other arm under your supporting arm. You may like to try using a pillow or cushion for additional arm support for yourself.

Here are a few examples of other positions that you may have heard about:
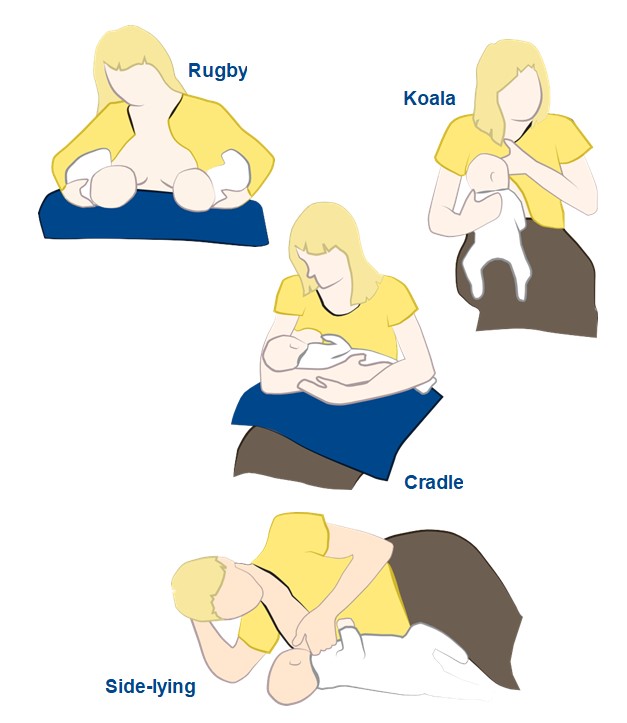
Check out our Padlet for more comfortable breastfeeding positions.
How milk is made
Your breasts have been producing small amounts of colostrum (first milk) from 16 weeks of pregnancy. After you have given birth, your milk making hormones are stimulated when your baby is held close and suckles. Milk is made on a supply and demand basis. Your baby needs to suckle often (between 8-12 times every 24 hours, plus cluster feed) in order for your milk production to increase. If your baby doesn’t suckle then we will support you to express. This will protect your milk supply until your baby is able to feed well. Milk production will reduce if it is not removed. The early days and weeks are very important for building your milk supply.
Colostrum treats and puddings!
We will encourage you to offer your baby regular colostrum treats, between feeds, until your milk comes in around day 3-4. This will help build your supply, keep baby satisfied, reduce jaundice by increasing stooling, reduce significant weight loss and prevent unnecessary formula supplementation.
Start straight after the first feed and try every 2-3 hours until your milk comes in. Babies love colostrum treats.
How to know that your baby is getting enough milk
- Most babies will feed between 8-12 times every 24 hours. If your baby is sleepy, try waking them up and offer your breasts every 2-3 hours.
- Your baby feeds between 5-40 minutes each feed.
- Your baby is calm and relaxed when feeding and content after feeding.
- Your baby has wet and dirty nappies appropriate for their age. This is important (see chart).
- Breastfeeding is comfortable for you.
- You notice your baby doing regular swallowing from around day 3-4 when your milk comes in.
Your baby’s nappies
- In the first 48 hours, your baby is likely to have only 2 or 3 wet nappies. Wet nappies should then start to become more frequent, with at least 6 every 24 hours from day 5 onwards.
- Your baby’s poo will change in colour, consistency and frequency:

- Breastmilk is a laxative and babies should poo at least twice a day for the first 6 weeks. If your breastfed baby does not poo for 24 hours please speak with your midwife or health visitor, as this may mean they aren’t getting enough milk.
- Most babies lose a little weight in the first few days. This is normal and to be expected. Most babies are back to their birth weight by day 14.
- Young babies need to wake and feed during the night. Their tummies are small and they are growing quickly. Try napping when your baby does during the day.
The Top-Up Trap
In the first few days, babies can be unsettled, fussy or sleepy. It is normal for babies to have periods of cluster feeding – particularly at night when the milk hormones are highest.
Sometimes, tired or concerned parents ask for formula supplements without realising the possible problems this can cause.
The ‘Top-Up Trap’ refers to the cycle of events that can start with the formula top-up. For example:
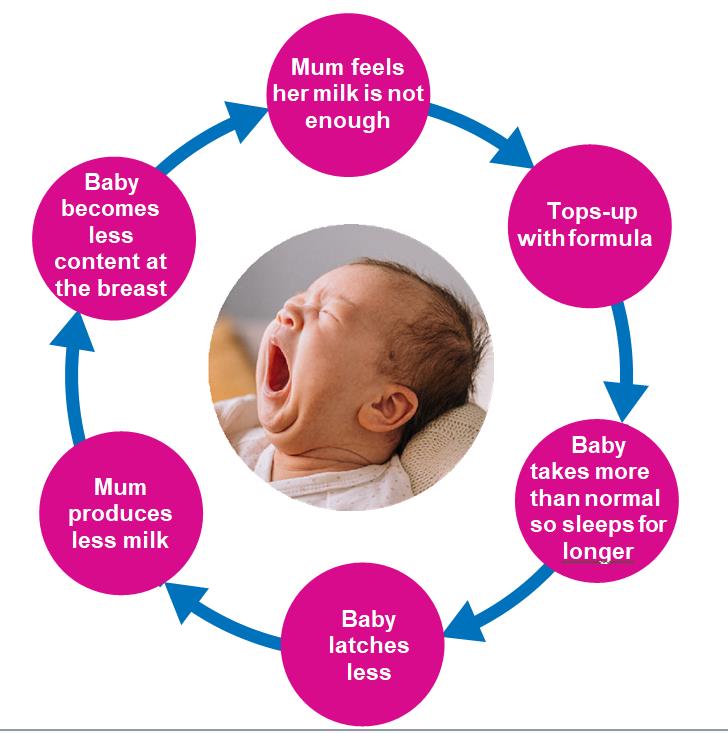
Issues with giving formula milk to a breastfed baby
- Increased risk of developing Cow’s Milk Protein Allergy (CMPA).
- Babies feed differently on a teat than they do a breast, this confusion can result in the baby latching less effectively.
- Reduced milk supply.
- Reduced confidence in milk supply.
- Formula feeds alter the bacteria in the baby’s gut. This may increase the risk of your baby developing infections.
Powdered Infant formula feeds should be prepared when needed, not in advance. Due to safety concerns, preparation machines are not advised.
Be advised
Feeding your baby exclusively human milk is recommended for the first 6 months, and then alongside solid foods for at least the first 2 years of life (World Health Organisation).
The role of the partner/co-parent
A partner’s support can be one of the most important factors in breastfeeding success.
How can a partner support breastfeeding?
- Give emotional and practical support: praising and encouraging breastfeeding can help to build their confidence.
- Be in charge of visitors: although everyone will want to meet the new baby, having lots of cuddles with others can be detrimental at the beginning and be exhausting for new mums!
- Feed the feeder! Always make sure there is a large glass of water and a snack next to your partner when they are breastfeeding.
- Enable your partner to meet their needs e.g. to shower, nap, exercise etc.
- Take over nappy-duty – particularly at night!
Responsive feeding
Breastfeeding your baby is more than food, it is also great for calming and soothing your baby.
It is important to respond to your baby’s early signs of hunger – crying is a late feeding cue!
Responsive breastfeeding is a two-way relationship between you and your baby that supports emotional wellbeing, not just food.
Reasons you might breastfeed your baby:
- Your breasts feel full.
- You want to sit down, relax and have a cuddle.
- Your baby is showing signs of hunger or thirst (feeding cues).
- Your baby seems distressed or needing comfort.
- Your baby is unwell.
Breastfed babies feed often, on average 8-12 times every 24 hours. Cluster feeding (wanting to feed more) is common during periods of growth. Always offer both breasts as your baby may want one or two each feed.
If feeding by bottle, hold your baby close, look in their eyes and limit the number of people feeding your baby in the early days. This will help your baby feel safe and secure. Learn more about responsive bottle feeding on page 23.
Early cues:
- Stirring
- Mouth opening
- Turning head / rooting
- Sucking on their hand
Late cues:
- Crying
- Agitated body movements
- Colouring turning red
Protection
Human milk protects both mother/birthing parent and baby. Here are 10 super facts about feeding your baby human milk.
- Human milk is alive! It changes throughout the day, months and years to meet your child’s needs.
- If your baby is unwell, your body will make substances in your milk, called antibodies, which will help make them better.
- Substances found only in human milk have the ability to kill cancerous cells.
- It contains stem cells – cells that create and repair the body.
- Your milk contains the “love hormone” oxytocin, causing relaxation and feelings of wellbeing in both the parent and child.
- Breastfeeding for at least 2 months halves the risk of Sudden Infant Death Syndrome.
- Human milk lowers your baby’s risk of allergies and illness. For example, chest, ear and stomach infections.
- Studies have shown breastfeeding for 6 months or longer reduces your baby’s chance of leukaemia by 20%!
- Breastfeeding reduces your chances of diabetes, heart issues, breast and ovarian cancer, osteoporosis and rheumatoid arthritis.
- Breastfeeding burns on average up to 500 calories a day!
Safety
Keeping your baby safe: food, family and environment.
Bottle feeding
Formula milk does not provide the same benefits for your baby that human milk can, such as protection against illness and infection. If you are unable to fully breastfeed, or choose not to, we will provide the support you need to bottle feed as safely as possible.
All brands of first milk formula milk must legally provide the same amount of nutrients, so it’s up to you which one you choose. The most expensive formula is no better for your baby than the cheapest!
Some parents will choose to give their expressed milk in a bottle. Human milk can be collected via hand expressing (see page 8-9) or using a manual or electric pump. If breastfeeding, it is advised to wait until this is established before introducing a bottle.
It is recommended that all bottle-fed babies are fed in a responsive way that involves following your baby’s cues (see page 19), rather than having a strict feeding schedule.
Feeding responsively also helps to reduce over-feeding as it allows them to pace the feed – over-feeding can lead to discomfort and pain, as well as obesity later on in life.
Be advised
You do not need to decide how you are going to feed your baby until after they are born. However, if you do bring formula into the hospital, please ensure it is a first milk formula in a ‘Ready to Feed’ carton.
Responsive bottle feeding
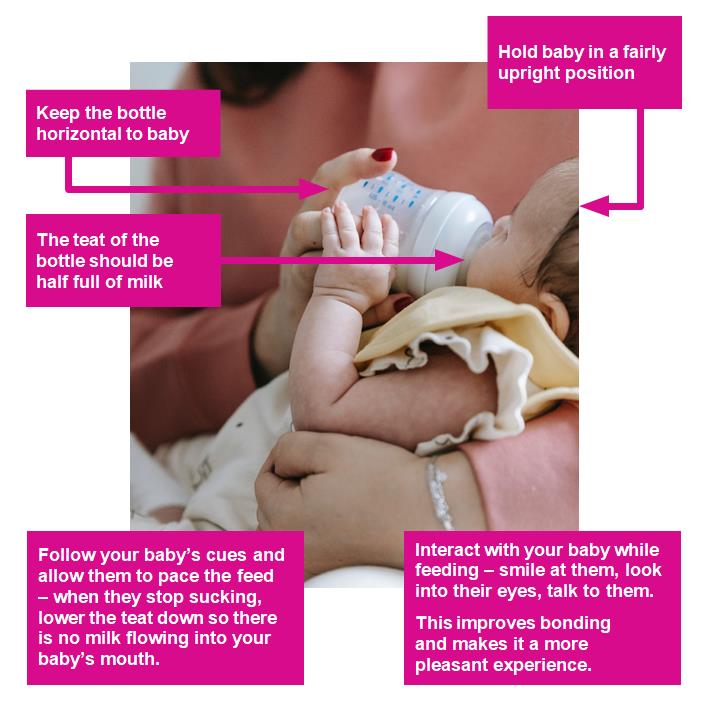
First stage milks only from birth to 1 year. Follow on or hungry baby milks are not recommended. Follow-on or hungry baby milks are not recommended. See our padlet for more info.
Safe sleeping
This advice has shown to reduce babies dying suddenly with no explanation (known as sudden infant death syndrome, SIDS or cot death).
- Always place your baby on their BACK for every sleep.
- Keep your baby smoke free before and after birth.
- Place your baby to sleep in a CLEAR, FLAT sleep space in the same room as you for every sleep for 6 months.
- Breastfeed your baby: evidence shows that Sudden Infant Death Syndrome (SIDS) risk is halved in babies who are breastfed for at least two months.
- Use a firm, flat, waterproof mattress in good condition.
Things to avoid:
- Never sleep on a sofa or in an armchair with your baby.
- Don’t sleep in the same bed as your baby if you smoke*, drink or take drugs or are extremely tired, if your baby was born prematurely or was of low birth-weight.
- Avoid letting your baby get too hot.
- Don’t cover your baby’s face or head while sleeping or use loose bedding.
Additional information
Our Flying Start: Feeding and Nurturing your Baby Padlet is packed with useful links, videos and resources such as:
- Bonding and brain development
- How to establish effective breastfeeding
- Breastfeeding challenges
- Medications and breastfeeding
- Expressing
- Formula feeding
- Where to find help and support
- Safe sleeping
- Mixed feeding
- Vitamin D guidance
- And much much more!
Being a new parent can be an amazing experience, but it can also be difficult. Young babies aren’t able to settle into routines. When babies are left alone to cry they release a stress hormone called cortisol. When babies are upset and crying they can’t soothe themselves, and they need their parents help to do this. All babies cry at times and some cry more than others.
- See the links to Building a Happy Baby and ICON crying advice on our Padlet.

Contact details and helplines
Establishing effective breastfeeding can take time and sometimes requires additional help and support.
If it is challenging for you, please ask for extra support. The first few weeks can be the hardest. We have extended teams of maternity staff, health visitors, breastfeeding drop-ins and volunteers trained to help you reach your feeding goals.
Infant feeding team
St Richards Hospital, Chichester
07808 099829
Worthing Hospital
07808 099816
Email
[email protected]
Royal Sussex County Hospital and Princess Royal Hospital Email:
[email protected]
Community midwife contact numbers
Royal Sussex County Hospital
01273 664794
Princess Royal Hospital
01444 448608
Worthing/ St Richards Hospital
01903 285269

Free trained breastfeeding volunteer helplines
NCT breastfeeding counsellors:
Call 0300 330 0700 available 8am to midnight.
National Breastfeeding Helpline:
0300 100 0212 available 9.30am to 9.30pm.
The ABM Breastfeeding Helpline number:
0300 330 5453 available 9.30am to 10.30pm.

To fill in the discharge table, please consult the PDF version of this booklet.
The information in this article is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.