Download and print as a PDF (1MB pdf)
On this page
- Journey countdown
- How does the gastric sleeve work?
- How much weight will I lose?
- My goals
- Planning and preparation
- Vitamin and mineral tablets
- Blood tests
- Pre-operative diet: milk diet
- Pre-operative diet: milk diet
- What will I eat after surgery?
- Eating rules
- Be aware
- Eating rules: long term goals
- Frequently asked questions
- Word dictionary
Journey countdown
Bariatric surgery permanently changes how you eat and drink. This information aims to provide you with essential information to achieve the best possible results. Please read it carefully.
Planning and preparation: Research, attend support groups, online forums, get questions for the team ready, stop smoking.
Paperwork: Complete questionnaire and online psychological assessment.
MDT Assessment: Day long appointment with the dietitian, anaesthetist, physician, nurse and surgeon.
Pre-op Assessment (2 to 3 months before surgery): Appointment with nurse and dietitian, blood test, measurements and MRSA screen.
1 to 2 weeks before surgery: Start Pre operative diet (milk diet).
Surgery: Hospital stay for 2 nights.
6 weeks post-op: Appointment with nurse.
3 months post-op: Appointment with dietitian.
6 months post-op: Appointment with dietitian.
12 months post-op (1 year): Appointment with dietitian and blood test.
18 months post-op: Appointment with dietitian.
24 months post-op (2 years): Appointment with dietitian and blood test.
You will be under our care for 2 years after your surgery. It is necessary to attend all follow up appointments.
Questions to ask your bariatric team at your next appointment (blank form for you to fill in).
How does the gastric sleeve work?
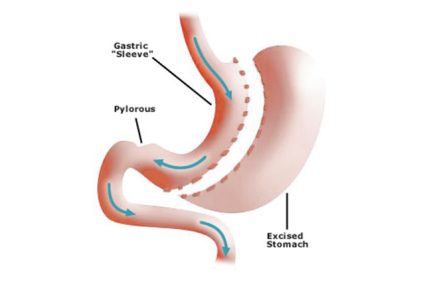
Restriction
The surgery reduces the size of your stomach. The stomach is divided to form a narrow tube, or ’sleeve’, which can only hold about 100mls. The remaining part of the stomach is removed.
If you pay attention to the signals, you will feel the sensation of fullness after a small amount of food. Over-eating can cause tummy discomfort and vomiting.
Hormones
The surgery affects the hormones that regulate your appetite. After surgery most patients feel less hungry and often forget to eat. If you do feel hunger, it is useful to establish if the hunger is actual physical hunger or emotional hunger. Even if you don’t feel hungry it is still important to eat. You should try to have something small and nutritious 3 to 6 times a day to keep
your mood and energy levels elevated.
If for any reason you cannot attend your appointment please call the bariatric office at the earliest opportunity.
How much weight will I lose?
Research shows that on average, you will lose 60% of your excess weight. This usually happens very quickly. You can lose up to 1 stone (6kg) per month for the first four months before the weight loss starts to slow down. In practice, weight loss is affected by age, activity level, dietary discipline and Basal Metabolic Rate (BMR). Some people lose more weight than expected, some lose less. It is difficult to predict.

To convert kg to stones and lbs, multiply by 2.2 and divide by 14.
My goals
This surgery is not just about weight loss. What do you want to achieve and change? Be realistic! (Blank page for you to fill in).
Planning and preparation
There are things that you can do now which will help you after your surgery.
• Read and research.
• Buy equipment e.g. blender, small food pots, side plate.
• Stop smoking.
• Think about exercise options e.g. investigate local gyms,swimming pools, classes, home workouts.
• Practice mindful eating – concentrate on your meal, chew well,avoid distractions.
• Consider who will do the cooking for the rest of the family whilst following the milk and puree diet.
• Think about how you will cope with eating food at work or social events.
• Build a support network e.g. friends, family, work colleagues,online forums, local support group.
• Take any recommended vitamin and mineral supplements.
This is usually a multivitamin and mineral tablet, 1 per day and Vitamin D3 1000IU, 1 per day.
• Take all your medication and treatments correctly.
Vitamin and mineral tablets
After surgery you will be unable to meet your vitamin and mineral needs with diet alone. This is because you will only be able to eat small quantities of food, you will not produce enough stomach acid for digestion and part of your digestive system is bypassed. This means you will need to take vitamin and mineral tablets for life.
You need:
• Multivitamin & Mineral.
• Calcium.
• Vitamin D3.
• Iron.
• Vitamin B12.
Please refer to ‘Vitamin & Minerals for life after bariatric surgery’.
Blood tests
You will have blood tests at least every year. This will check kidney and liver function, bone health and vitamin and mineral levels.
Pre-operative diet: milk diet
Why do I need to follow this diet?
• This diet shrinks the size of your liver before surgery. This allows the surgeon access to your stomach and reduces the risk of damage to your liver during the operation.
• This diet starts your weight loss journey.
How long do I need to follow the diet?
The length of time you need to follow the diet depends on your BMI and liver health. It is usually for a maximum of 2 weeks.
Start of milk diet
From midnight, night before surgery: clear fluids e.g. water, black tea, black coffee, squash.
06:30 / 11.30 (depends on the time of your operation): Nil by mouth.
What is the risk of not following the diet?
Your surgery will be abandoned if the liver is too large and obscures the surgeons view of the stomach.
Do you have diabetes?
Please inform your diabetes team that you will only be taking 120g of carbohydrate per day. Your diabetes team will advise you on any changes to your diabetes medications and/or adjustments to your dose of insulin/s. If you take insulin or oral medications that can cause hypos, you need to check your blood sugar levels at least 4 times per day.
Constipation
The most common side effect of the diet is constipation. We recommend you take milk of magnesia or Benefiber or Movicol to relieve these symptoms. Please try not to arrive for surgery
constipated!
Pre-operative diet: milk diet
Every day you must have the following:
• 4 pints (2 litres) of either semi-skimmed cow’s milk, lactose free milk or soya original. Please note that alternative milks such as oat, almond or rice milk are not suitable.
• At least 2 pints (1 litre) of calorie free fluid.
• 1 salty drink e.g. Marmite, Bovril, stock cube or 1 tsp salt in squash.
• 1 multivitamin and mineral tablet e.g. Sanatogen A-Z or Tesco A-Z.
• No food.
Allowed drinks
• Tea, coffee or herbal tea.
• Water.
• No added sugar squash.
• No added sugar Crusha or Okcal syrups can be added to milk.
Allowed extras
• 1 sachet or 5 x 115g pots of ready to eat sugar free jelly per day (1 pint).
• Chewing gum (maximum 3 pieces per day).
Tips
• Keep your milk separate from anyone else’s at home.
• Use sweeteners instead of sugar in tea and coffee.
• Ensure you have everything you need before you start.
• Plan your routine for fitting in all of your fluids.
• Consider how the milk diet may affect your family and what support you will need e.g. who will do the cooking.
• Think about how you might cope with following the milk diet at work or special occasions.
• Remove all tempting foods from the house as much as possible.
This diet is preparation for surgery, not for weight loss.
It should only be used under supervision from your dietitian for a maximum of 2 weeks.
Please contact the dietitian if you suffer any side effects from this diet.
What will I eat after surgery?
Textures need to be introduced gradually to allow for healing and your new stomach pouch to adapt.
Stage 1: pureed consistency (weeks 1 to 4)
No lumps, smooth like the consistency of a yoghurt
• Do not eat and drink more than 2tbsp or 100-200ml at a time.
• Blenders or liquidisers and sieves are necessary.
• Add a liquid to help achieve a smooth food consistency e.g.tomato puree, gravy, stock or milk.
• Puree the protein component separately from the vegetable or potato to give you different flavours on your plate.
• You may not feel up to cooking after your operation. Be prepared by cooking, blending and freezing foods before your surgery.
• Freeze in ice cube trays which helps you get familiar with portion sizes without causing waste.
Stage 2: mashed/crunchy consistency (4 to 8 weeks)
Bridge between pureed foods and normal textures
• Practice the eating behaviours that will result in a good long-term weight loss.
• If you experience discomfort, try to work out why: did you eat too much, eat too fast, or didn’t chew thoroughly enough?
• Initially foods will be better tolerated if they are soft and wet. Adding gravy or sauces can help
• The fork test can be used to check the texture. If your fork passes easily through the food, it is the right texture for stage 2. If you have to force a fork through it is probably a stage 3 food and best avoided at this stage.
Stage 3: normal consistency (8 to 12 weeks)
It is now safe to start experimenting with different textured foods
• There will still be some foods that you cannot tolerate. Bread, pasta, rice and dry meats are the usual problem foods. Take things slowly. Add one new food at a time.
• From about 10-12 weeks you can try salads.
• Try to avoid soft/sloppy food as this will result in overeating.
• Please experiment carefully to see what you can tolerate. This varies from person to person. Foods that you could not manage at the beginning will be tolerated at a later date. Try again 1 to 2 weeks later.
Weeks 1 to 4 puree
Breakfast
- 2 to 4 tbsp. Weetabix or Ready Brek.
Lunch
- 100 to 200mls soup with protein
- 2 to 4 tbsp. tinned spaghetti.
Dinner: A balanced meal of protein, vegetable and potato.
- 1 to 2 tbsp. meat / fish.
- ½ -1 tbsp. vegetables.
- ½ -1 tbsp. potato.
Snacks
- 2 to 4 tbsp. of yoghurt.
- Custard (low sugar).
- Pureed fruit.
- Rice pudding (low sugar).
- Hummus.
- Peanut butter.
- Pate.
- 100mls milky drink.
Weeks 4 to 8 mashed / crunchy
Breakfast
- ¾ Weetabix.
- Scrambled egg on ½ slice toast.
- 4 tbsp. cornflakes.
Lunch
- Baked beans.
- Ravioli.
- Omelette with cheese.
- ½ Jacket potato with tuna or cheese.
- Chunky soup.
- Cauliflower cheese.
Dinner: A balanced meal of protein, vegetable and potato.
- 4 tbsp. meat / fish casserole.
- 1 tbsp. soft vegetables.
- 1 tbsp. mashed potato.
Snacks
- Soft fruit (no skins).
- Yoghurt.
- Soft cheese and 1 to 2 crackers.
- Pate and 1 to 2 melba toast.
- Hummus and 1 to 2 Rice cakes.
Weeks 8+ normal
Breakfast
- 1 Weetabix
- Any no added sugar breakfast cereal.
- ½ slice toast and poached egg.
Lunch
- Jacket potato with beans / tuna / cheese / prawns.
- Salad with egg / beans / meat / fish.
- Sardines on toast; Pitta with cheese and salad; Wrap with chicken and salad; ½ toasted sandwich.
Dinner: A balanced meal of protein, vegetable and potato.
- Fishcakes with potato wedges and vegetables.
- Roast meat with potatoes and vegetables.
- Chicken curry and rice.
Snacks
- Fruit.
- Small handful of nuts.
Eating rules
How you eat and drink is just as important as what you eat and drink.
Speed
Eat slowly. A meal should last 20 to 30 minutes. Shorter than this, you are eating too quickly. Longer than this, you are trying to eat too much food. Eating fast can lead to pain, discomfort and regurgitation.
Chew
Normally your stomach churns food to break it down for digestion. Now your chewing must do that job. Chew 20 times per bite until smooth with no lumps before swallowing. Do not gulp when swallowing liquid as this will also cause pain.
Calm atmosphere
Make time for your meals and snacks, create a calm environment with no distractions. Awareness helps you to eat correctly. Take your time to eat as it should be an enjoyable experience and it also encourages a feeling of fullness.
Volume and meal pattern
The volume of food and fluid your stomach can tolerate will be considerably reduced. At first, you will only manage about 2 tbsp. or 100 to 200mls at a time. Try to eat 6 times a day for the first few weeks after surgery. Ensure a regular eating pattern and avoid long periods without food.
As the months go by, you will be able to eat more at each meal. It is important to listen to your body and stop eating when you are full. Over-eating can cause you to be sick or to feel uncomfortable. This behaviour may result in poor long term weight loss.
By 6 months after surgery, you will be able to eat a tea plate sized portion. It is important that portions do not increase beyond this. At this time, a typical meal pattern would be 3 main meals and 2 to 3 small snacks a day. Eating well takes careful planning. Be aware of inappropriate snacks creeping in.
Protein first
Rapid weight loss can cause loss of muscle mass, weakness and reduced immune function. Protein is one of the building blocks for every cell in your body and needs to be the main component of your diet, especially in the early stages.
Make sure you eat your protein food first. Good protein sources include; fish, chicken, beef, lamb, pork, eggs, pulses (peas, beans, lentils), nuts, cheese, milk, yoghurt, fromage frais, soya alternatives, tofu and Quorn.
Sugar and dumping syndrome
Dumping syndrome is caused by food moving quickly through the gut. Sugar is absorbed very quickly and causes a rapid swing in your blood sugar levels. The symptoms are nausea, vomiting, sweating, dizziness and diarrhoea. If you have one of these events take a rest, then try to work out what caused it. This will help prevent it from happening again. In order to avoid dumping syndrome avoid high sugar foods such as chocolates, sweets, cakes, desserts, biscuits and fruit juices. There are hidden sugars in lots of foods so it is sensible to check food labels. As a guide, avoid foods with more than 5g sugar per 100g in the food or drink.
Fluids
Dehydration can cause low energy levels, headaches and dizziness. Aim for a minimum of 2 litres per day (8 cups). Try to sip slowly throughout the day. You will not be able to gulp drinks when thirsty or in a hurry.
Avoid drinking and eating at the same time, you should not drink 30 minutes before or after food. Alcohol is not recommended during the first year after surgery because of its high calorie content and gassy drinks will not be tolerated well. You are likely to feel the effects of alcohol quickly. Drinking alcohol may impact on you achieving your goals.
Good options:
- Water.
- Tea or coffee (can add sweetener).
- Sugar free squash.
- Diluted fruit juice (maximum 1 glass per day).
- Milk.
- Herbal tea.
- Sugar free jelly.
- Ice pops made from sugar free squash.
Poor options:
- High calorie lattes.
- Sugary flavoured water.
- Alcohol.
- Fizzy drinks.
- Sparkling water.
Be aware
Fertility and pregnancy
Many obese women don’t ovulate regularly and consider themselves infertile. This can change with weight loss. For this reason female patients should consider which form of contraception
they wish to use. The oral contraceptive pill is not be reliable after bypass surgery and we recommend patients use an alternative form of contraception such as a depo injection, barrier methods or a coil. Your GP should be able to advise you appropriately. Pregnancy should be avoided for the first year after surgery.
Depression and eating disorders
Surgery is challenging. Some people suffer psychologically after the surgery particularly in dealing with their new body image and emotional relationship with food. People with underlying eating disorders may develop new eating disorders. Please discuss these
challenges with your team who can direct you to the best support.
Hair loss
Surgery and rapid weight loss can result in hair loss 3 to 6 months after surgery. This usually lasts for around 3 months but it can take some time for your hair to recover. The dietitian will monitor your food intake to ensure you are supporting your hair re-growth. Taking your recommended vitamins is essential, but there is no need to buy any specific supplements for hair re growth.
Bowels
Your bowel habit can alter after surgery. You may have diarrhoea as you are malabsorbing nutrients and the flow of food through the system is much quicker. You may have constipation if your fluid intake is low, your fibre intake is low, your body is used to requiring laxatives or you are inactive. Please discuss with your team if you have any concerns.
Exercise
Exercise will help maintain muscle tone, accelerate weight loss and improve mental health. Try to start with a small goal e.g. a daily walking plan. Walking is beneficial as it is a weight bearing exercise and can help protect your bones from osteoporosis. Over time, you will be able to build up your stamina and move on to other forms of activity. If you suffer with joint pain then water based exercises such as swimming or water aerobics, which puts less pressure on the joints, may be more suitable.
Weight regain
It is estimated that 15 to 35% of patients do not achieve satisfactory weight loss or will regain weight. Conditions like diabetes, sleep apnoea and high blood pressure which went into remission can become a problem again. To give yourself the best opportunity to achieve your goals be well prepared before surgery, attend all appointments and follow the advice of your bariatric team. This surgery does not ‘cure’ weight issues. It will always need monitoring and discipline.
Eating rules: long term goals
• Eat regularly, at least 3 meals a day.
• Always eat breakfast.
• Balanced main meals: include protein AND carbohydrate AND vegetables / salad.
Protein: eat first: Meat, fish, milk, cheese, yoghurts, egg, Quorn, tofu, nuts, lentils, beans.
Vegetables / Salad / Fruit: a portion is a handful: Aim for a mixture of textures and colours.
Carbohydrate: choose high fibre, low sugar options: Potatoes, pasta,rice, couscous, bread, crackers.
• Eat slowly. Take 20 to 30 minutes to eat a meal.
• Take small bites. Your mouthful should be the size of a 20p piece.
• Chew really well before swallowing. Chew until smooth with no lumps and then swallow.
• Put your spoon down between each mouthful.
• Stop eating before you are too full. Learn to detect your own signals of ‘too much.’ Usual signs are a pain in the shoulder or upper chest, nausea or the production of saliva.
• Use a small plate to control portion sizes. Smaller cutlery also helps.
• Do not leave food on a plate to return to it later. Clear it away.
• Sip fluids slowly rather than taking large mouthfuls.
• Mindful eating: concentrate on your meal rather than watching television or working while eating.
• Avoid simple sugars. Remember honey, jam, sucrose, lactose and fructose are all forms of sugar.
• Do not add lots of gravy or sauce to ‘help food get down’. Your portion size will grow too large and you can regain weight.
• Weigh yourself regularly (but no more than once a week).
• Be as active as you can every day.
• Take your vitamin and mineral tablets.
• Make sure you have a blood test every year.
• If you are not happy with your weight changes, go back to basics and start a food diary.
Frequently asked questions
I have a problem being sick after eating. What do I do?
It might take time for you to put the eating rules into practice. If you produce white froth or regurgitate food consider the following:
• Did I eat too quickly?
• Did I chew it well enough?
• Was it too soon after surgery to have the food I was eating?
• Did I eat too much?
If you experience persistent vomiting contact your bariatric team for advice.
What should I do if I have a problem with nausea?
Make sure your medications have been reviewed by your GP. Do not skip meals. Eat small amounts 6 times a day.
What can I do if I get constipated?
If you get constipated, first check that you are drinking enough fluids and eating enough fibre. You can take a laxative if constipation is a problem. For example Benefiber, Movicol or lactulose, but you must drink enough fluids for the laxatives to work. It is also important to be as active as possible.
What can I do if I get diarrhoea?
Do you have a bug? Have you recently taken antibiotics? Have you eaten food high in sugar that gave you dumping syndrome? If you experience persistent diarrhoea, contact your Bariatric team for advice.
Do I have to follow the puree diet for 4 weeks?
Yes. Your gut is healing from the surgery during this stage. It is important to be confident with each stage before you progress onto the next.
Can I eat baby food on the puree stage?
No. Baby food does not provide adequate nutrition for adults.
Should I take protein shakes?
No. You should eat your calories, not drink them.
Why haven’t I lost any weight?
Do not weigh yourself every day. Our advice is to wait until your 6 week appointment with the nurse. In the weeks following your surgery your body is recovering. You might not lose weight every week. Follow the advice in this booklet and you will lose weight. Make sure you are eating 6 times a day and drinking enough fluid.
How much can I eat?
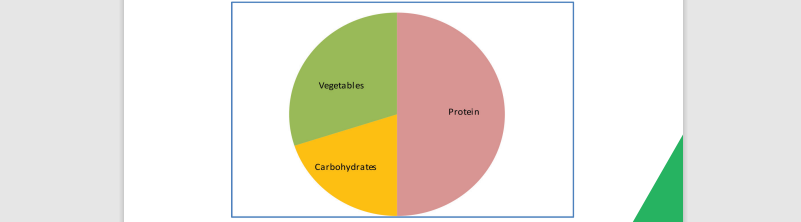
Your portion sizes increase gradually from 2tbsp per meal to a side plate over the first 6 months. It is important to learn when to stop eating and you should be guided by signals from your body with this. It can be difficult not to finish everything on your plate, remember to serve small portions to avoid battling with food waste. As a general guide, main meals should be the size of a side plate (this is about the size of your hand span) and include protein, vegetables and starchy carbohydrates in the proportions shown below.
Word dictionary
Gastric: Stomach.
Laparoscopic: Keyhole, small cuts.
MDT: Multidisciplinary Team group of health care professionals.
Pre-op: Before your operation.
Post-op: After your operation.
Surgery: Operation.
GP: General Practitioner (Doctor).
Dietitian: Health care professional who translates nutrition science to provide advise about food and treat and prevent nutrition related problems.
Anaesthetist: Medical doctor trained to give anaesthetics.
Physician: Medical doctor qualified to practice medicine and specialises in diagnosis and medical treatment.
Surgeon: Medical doctor qualified to practice surgery.
Abdomen: Belly, part of the body that contains your gut.
IBW: Ideal Body Weight, healthy weight for your height.
EBW: Excess Body Weight, any additional weight over your ideal body weight.
BMR: Basal Metabolic Rate, energy you burn when resting.
Ovulation: Part of the female menstrual cycle where an egg is released in the ovary.
U&E: Urea & Electrolytes.
LFT: Liver Function Test.
FBC: Full Blood Count.
PTH: Parathyroid Hormone.
TBSP: Tablespoon (15mls).
Contact us
Bariatric Surgery Service
St Richard’s Hospital
Spitalfield Lane
Chichester
West Sussex
PO19 6SE
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.