Download and print as a PDF (436kB pdf)
On this page
- What is Viral Induced Wheeze? (VIW)
- Does this mean my child has Asthma?
- How is Viral Induced Wheeze treated?
- Are there any side effects of the treatment?
- When can my child go home?
- What should I do next time?
- When should I come back to hospital?
- If you have any further questions about Viral Induced Wheeze
What is Viral Induced Wheeze? (VIW)
In young children, wheezing is usually caused by a cough and cold virus. The virus causes inflammation and narrowing of the airways, which results in the high pitched
whistling noise characteristic of wheeze.
Symptoms can include:
- Cough and cold
- Wheezing
- Difficulty in breathing
- Raised temperature
- Difficulty in feeding
Does this mean my child has Asthma?
Not necessarily. Whilst the symptoms can be similar, VIW is a different
illness to asthma. Intermittent wheezing with colds is quite common in younger children
and only a small proportion go on to develop asthma. The risk however is higher if there
is a family history of asthma, eczema and / or hayfever.
How is Viral Induced Wheeze treated?
Medications called bronchodilators or ‘relievers’ are used to open up the airways.
These are usually given through a blue inhaler, sometimes called a ‘puffer’, and a spacer device. The reliever inhaler that we use is called Salbutamol (Ventolin).
When your child first arrives at the hospital they may be given multiple doses of inhalers.
This is routine treatment, and the amount given will be reduced as your child gets better.
Other treatments that your child may need:
Dexamethasone or prednisolone: steroid medication given by mouth, which will help to
reduce inflammation in your child’s airways.
Oxygen: if your child needs oxygen they will have to stay in hospital. Oxygen or air may sometimes be given through devices called ‘Optiflow™’ or ‘Vapotherm®’. These can help your child’s breathing by delivering warm, wet air through small plastic pipes that sit in your child’s nostrils.
Intravenous medication: if your child is not getting better they may need to have reliever medications through a drip.
Antibiotics are rarely used in the treatment of Viral Induced Wheeze because they are ineffective against viruses.
Are there any side effects of the treatment?
The inhalers are safe and effective, however they can make your child’s heart beat faster
and can sometimes make them feel ‘shaky’ or give them a headache. This will not harm
your child and will get better as the treatment is reduced.
Steroid medications are very unlikely to produce any side-effects or long term problems at the doses used.
When can my child go home?
Your child will need to stay in hospital until you and the hospital team feel that they
are better. This is usually when your child is only requiring the inhalers every 4 hours,
and does not need oxygen. This can take 1 to 2 days or even longer, depending on how
quickly your child recovers.
Treatment at home after leaving hospital:
Your child should continue to have the reliever inhaler regularly until they are better. Give them up to 4 puffs of Salbutamol (Ventolin) every 4 hours. If you feel that your child is not improving within a few days, please arrange to get them checked over by their GP.
How to use the inhaler and spacer:
- Shake the inhaler well and remove cap. Fit the inhaler into the opening at the end of the spacer.
- Place the mask over your child’s nose and mouth. Ensure there is a good seal around the mask or mouthpiece.
- Press the inhaler once and slowly count to 10 for each puff.
- Shake the inhaler after every other puff.
Repeat for each dose of medicine.
Only put one puff of medicine into the spacer at a time as your child may receive the incorrect dose otherwise.
Always use the inhaler with a spacer and mask.
What should I do next time?
Some children have repeated episodes of wheezing with coughs and colds. The next time your child gets a cough and cold it’s important to use the inhaler early as it will have a better effect.
At the beginning of a cold, give 2 to 4 puffs of Salbutamol (Ventolin) through a spacer and mask every 4 hours for a few days.
When should I come back to hospital?
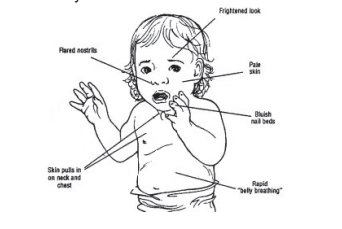
If the reliever inhaler is not lasting for 4 hours, or your child is / has:
Blue lips
Fast and laboured breathing
Grunting noises when breathing
Coughing and wheezing a lot
Too breathless to drink or to talk in sentences
Give 10 puffs of Salbutamol (Ventolin) through a spacer and mask and seek urgent medical attention.
If you have any further questions about Viral Induced Wheeze
Please telephone 01273 696955 and ask for the Children’s Respiratory Nurse Specialist. Office hours only.
Other useful numbers
Practice Plus (Brighton walk-in centre / GP service)
0300 130 3333
Open 7 days a week including bank holidays
8:00 am to 8:00 pm
Out of Hours GP Service or advice ring
NHS 111
This leaflet is intended for patients receiving care in Brighton & Hove or Haywards Heath
The information in this leaflet is for guidance purposes only and is in no way intended to replace professional clinical advice by a qualified practitioner.