Download and print as a PDF (6MB pdf)
On this page
- Welcome to the Trevor Mann Baby Unit
- What you can expect from our staff
- What we expect of parents
- Handover Times
- Medical ward rounds
- The nurseries
- Infection prevention
- Visiting
- Quiet time
- Unit facilities
- Confidentiality
- Safeguarding children
- Consent
- Car parking
- Safety and security
- Smoking
- Family integrated care
- Developmental care
- Kangaroo care
- Physiotherapy
- Feeding your baby
- Speech and language therapist (SALT)
- Ophthalmology
- The neonatal transfer service
- Preparation for home
- The neonatal outreach team
- Financial support
- Charities and other support available
- Counselling service
- Spiritual wellbeing
- vCreate
- Feedback and complaints
- The local area
- Frequently asked questions
- Appendix
Welcome to the Trevor Mann Baby Unit
Congratulations on the birth of your baby!
We realise that this is a difficult time for you, but we hope that this information will help reduce some of the stress involved in having your baby on the Trevor Mann Baby Unit [TMBU].
We are a surgical Neonatal Intensive Care Unit [NICU] that provides specialist care for babies who are unwell. This includes babies that are born prematurely and term babies who are unwell. As a surgical unit, your baby may have been transferred to our unit because they require surgery. Our NICU has allthe necessary facilities and staffing to deliver high quality and up-to-date intensive care to newborn babies and supportive care to babies and parents during the stages of recovery and growth.
Your baby is here because they need extra medical, surgical and nursing care. If your baby has come to TMBU because they require specialist care, our aim is to transfer your baby back to your booking hospital or one closer to home as soon as is appropriate.
We are continually involved in local, national and international research projects. As a result of many parents consenting to their babies’ taking part in such research, we have been able
to constantly improve neonatal care. If your baby is a suitable candidate for one of the research projects we are involved in, a member of the research team will discuss the option of participation. It is completely voluntary, but we will give you all the information so that you are able to make an informed decision.
This welcome booklet will provide you with an overview of our neonatal unit and the care we provide. We hope you will use it as a reference guide throughout your neonatal journey, alongside the unit app and staff support
What you can expect from our staff
• We are here to help and support you as a family, keeping you updated on the progress of your baby.
• We will be honest and open, including you as partners in your baby’s care.
• Our aim is for you to be confident and skilled in caring for your baby while on the neonatal unit.
What we expect of parents
• We ask that you work with us as partners in the care of your baby. This means being as present as possible to care for your baby, attending ward round discussions and having skin-to-skin cuddles with your baby when appropriate.
• When you feel ready and able to, you follow and complete the ‘Steps to Home’ booklet during your neonatal journey in preparation for discharge home. You can start this from
admission and should help you be more involved in your baby’s care.
• To bring in supplies for your baby such as nappies, nappy bags, cotton wool,and cotton buds.
• Follow our unit guidelines and policies throughout your stay, such as visiting and infection prevention measures (you will find more information about this in this welcome guide).
Main hospital switchboard
Nursery three direct phone
01273 696995
Ext. 63948
Princess Royal Special Care Baby Unit
Outpatient appointments
01273 696955
Ext. 64195/64188
Handover Times
Medical ward rounds
The nurseries
Infection prevention
Visiting
Quiet time
Unit facilities
Confidentiality
Safeguarding children
Consent
Car parking
Safety and security
Smoking
Family integrated care
Developmental care
Kangaroo care
Physiotherapy
Feeding your baby
Speech and language therapist (SALT)
Ophthalmology
The neonatal transfer service
Preparation for home
The neonatal outreach team
Financial support
Charities and other support available
Counselling service
Spiritual wellbeing
vCreate
Feedback and complaints
The local area
Frequently asked questions
Appendix
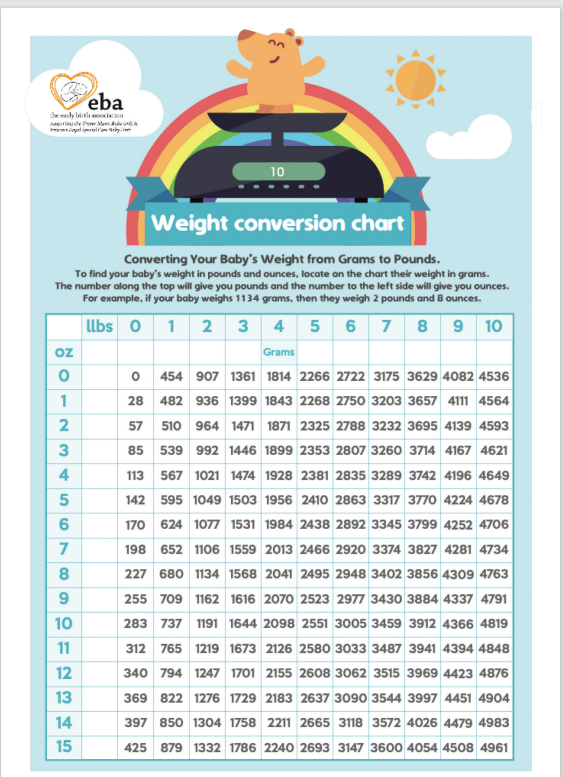
• Weight Conversion Chart
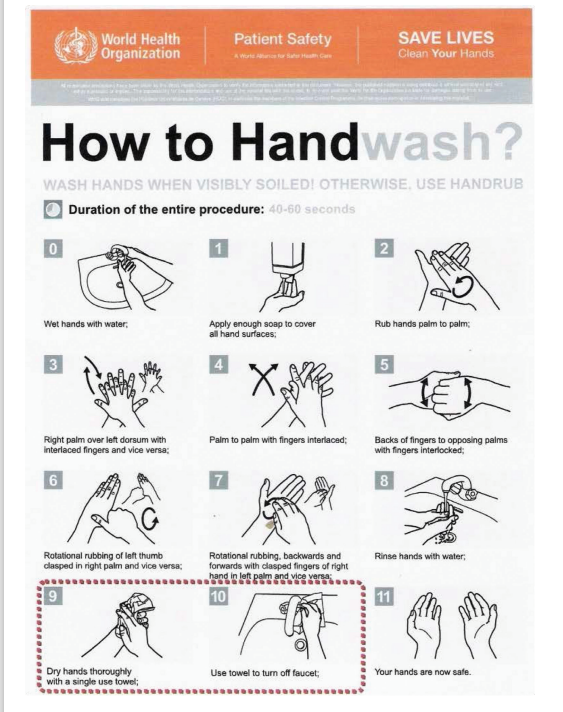
• WHO Hand Washing Technique
• Words You May Hear on the Unit
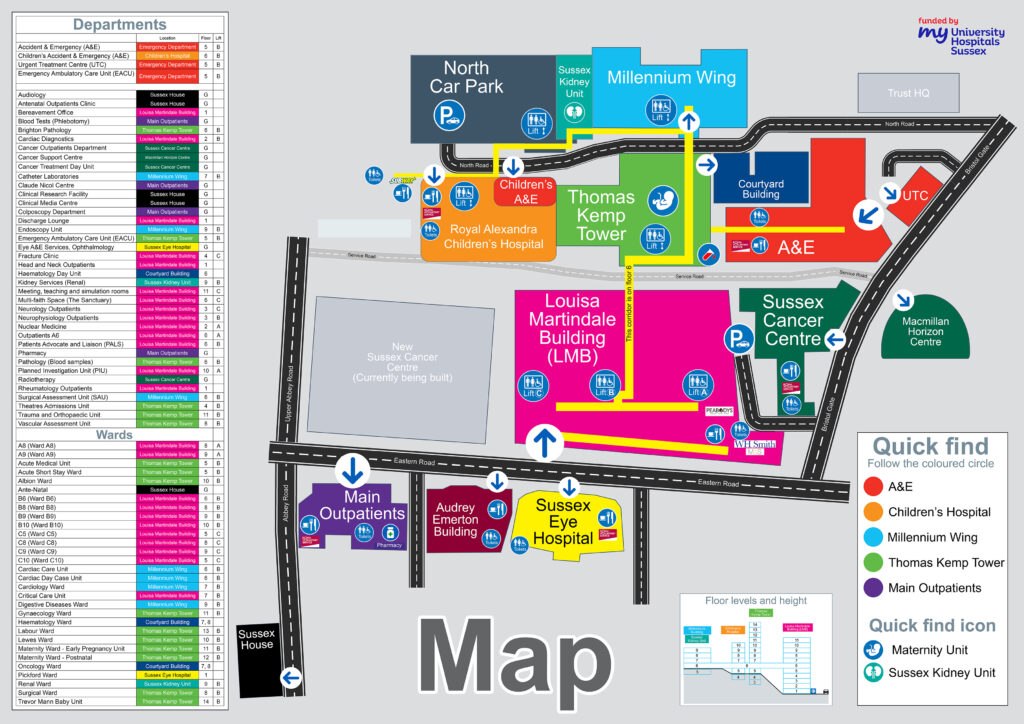
• Royal Sussex County Hospital Map
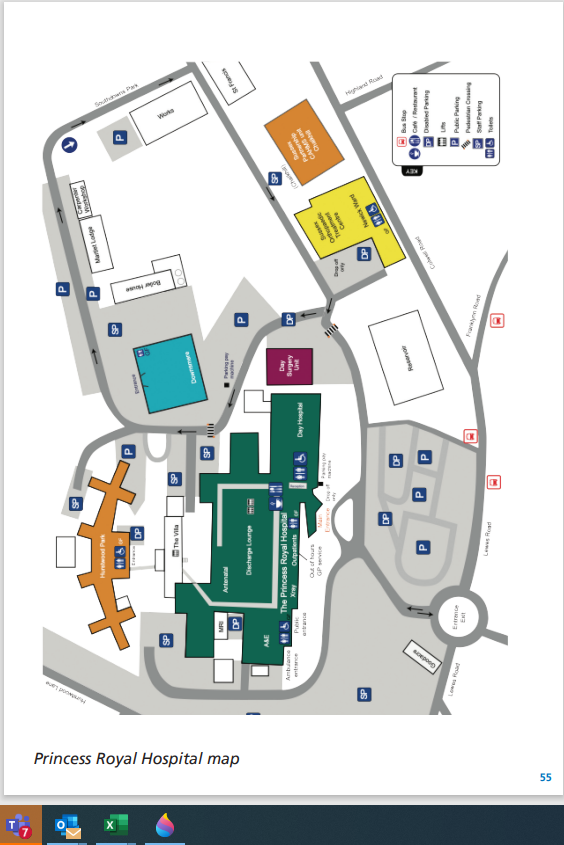
• Princess Royal Hospital Map

This leaflet is intended for patients receiving care in Brighton & Hove or Haywards Heath.
The information in this leaflet is for guidance purposes only and is in no way intended to replace the professional clinical advice by a qualified practitioner.